Pressure injuries—also known as pressure ulcers, decubitus ulcers, or bedsores—are localized damage to the skin and underlying tissue, primarily caused by prolonged pressure or pressure in combination with shear. They are a major concern for patients with limited mobility, especially in hospitals, long-term care facilities, and at home. Beyond the physical toll on patients, pressure injuries exact a heavy cost on healthcare systems and society at large. This document explores the true cost of pressure injuries and outlines comprehensive strategies for their prevention and management.
The Scope and Impact of Pressure Injuries
Pressure injuries are far more than a superficial wound. They represent a complex clinical challenge with multidimensional impacts:
- Incidence and Prevalence: Pressure injuries affect millions worldwide. In the United States alone, it is estimated that over 2.5 million patients develop pressure injuries annually, and the global burden is significant.
- Patient Populations: Highest risk groups include individuals who are elderly, immobilized, post-surgical, or have chronic illnesses such as diabetes or vascular disease.
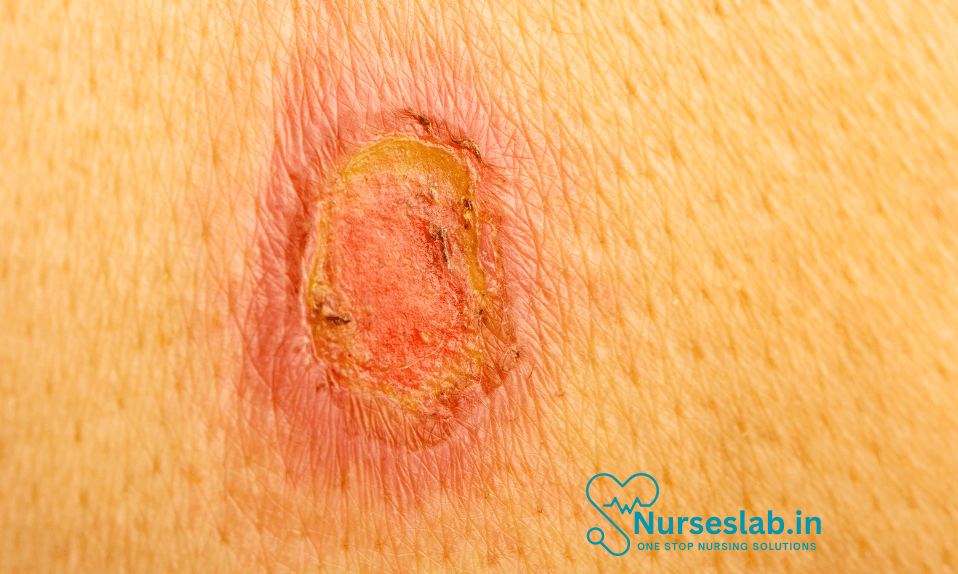
- Severity: Injuries range from mild erythema (Stage I) to deep tissue involvement and exposed bone (Stage IV), and can lead to serious complications such as sepsis, osteomyelitis, and death.
The True Cost of Pressure Injuries
The cost of pressure injuries is multifaceted, encompassing economic, clinical, and human dimensions.
Economic Costs
- Direct Medical Costs: Treating pressure injuries is expensive. Costs include wound care supplies, medications, advanced dressings, negative pressure therapies, surgical interventions, and extended hospital stays. In the U.S., the estimated annual cost for treatment ranges from $9.1 to $11.6 billion.
- Indirect Costs: These include lost productivity for patients and caregivers, litigation, and increased insurance premiums. Institutions may face financial penalties for high rates of hospital-acquired pressure injuries, as some insurers do not reimburse for their treatment if acquired during hospitalization.
- Resource Utilization: Pressure injuries consume significant nursing time, which could otherwise be allocated to other patient care activities. Each wound dressing change, assessment, and documentation adds to the workload.
Clinical Costs
- Increased Morbidity and Mortality: Pressure injuries are associated with a higher risk of infection, delayed recovery, and increased length of stay. The presence of a pressure injury can double the risk of mortality in some populations, such as the elderly.
- Complications: These wounds may lead to severe complications, including cellulitis, osteomyelitis, and systemic infection (sepsis), requiring intensive treatment and raising the risk of death.
Human and Social Costs
- Pain and Suffering: Pressure injuries cause significant pain, discomfort, and distress. They affect mobility, sleep, independence, and overall quality of life.
- Psychosocial Impact: Patients may experience depression, anxiety, social isolation, and a diminished sense of dignity.
- Caregiver Burden: Family members and professional caregivers face increased workloads, emotional stress, and financial strain when managing pressure injuries.
Prevention of Pressure Injuries
Prevention is the most effective strategy in reducing the incidence and cost of pressure injuries. Evidence-based practices include:
Risk Assessment
- Use validated tools such as the Braden Scale or Norton Scale to assess risk upon admission and regularly thereafter.
- Identify at-risk individuals early and implement targeted prevention plans.
Skin Care and Inspection
- Perform daily skin inspections, especially over bony prominences (sacrum, heels, elbows, hips, etc.).
- Maintain clean, dry, and moisturized skin. Promptly address incontinence to reduce moisture-related skin damage.
Pressure Redistribution
- Reposition patients at least every two hours, or more frequently for high-risk individuals.
- Utilize specialized support surfaces such as pressure-relieving mattresses, overlays, and cushions.
- Use heel protectors and offloading devices for vulnerable areas.
Nutrition and Hydration
- Ensure adequate caloric and protein intake to support skin integrity and healing. Collaborate with dietitians for patients at risk of malnutrition.
- Promote regular hydration to maintain skin turgor and elasticity.
Education and Training
- Educate healthcare staff, patients, and caregivers about risk factors, prevention strategies, and early signs of pressure injury.
- Foster a culture of vigilance and accountability around pressure injury prevention in all care settings.
Mobilization
- Encourage and assist patients to change position, mobilize, and participate in physical therapy as able.
Management of Pressure Injuries
Despite best prevention efforts, some pressure injuries will still occur. Effective management minimizes complications and promotes healing.
Assessment and Staging
- Correctly identify the stage of the pressure injury to guide treatment. Document wound size, depth, exudate, appearance, and signs of infection.
Cleaning and Debridement
- Irrigate wounds with saline or appropriate cleansers to remove debris and bacteria.
- Debride necrotic tissue, using surgical, enzymatic, or autolytic methods as appropriate for the patient’s condition.
Dressings and Wound Care
- Select dressings that maintain a moist healing environment, manage exudate, and protect from infection. Choices include foams, hydrocolloids, hydrogels, alginates, and antimicrobial dressings.
- Change dressings according to manufacturer recommendations and wound status.
Infection Control
- Monitor for local and systemic signs of infection: increased redness, warmth, purulent discharge, fever, or malaise.
- Initiate appropriate topical or systemic antibiotics when infection is suspected or confirmed.
Pain Management
- Administer analgesics as needed before dressing changes or procedures.
- Consider non-pharmacological interventions such as repositioning, relaxation techniques, and psychological support.
Advanced Therapies
- For non-healing wounds, consider advanced modalities such as negative pressure wound therapy, biologic dressings, or surgical intervention (skin grafts, flaps).
- Consult wound care specialists and multidisciplinary teams as needed.
Comprehensive Care Planning
- Engage in regular reassessment and adjust interventions based on wound progress and patient response.
- Integrate pressure injury management into holistic care plans that address underlying comorbidities, functional status, and patient/family goals.
REFERENCES
- Singh C, Shoqirat N, Thorpe L, Villaneuva S. Sustainable pressure injury prevention. BMJ Open Qual. 2023 Jun;12(2):e002248. https://pmc.ncbi.nlm.nih.gov/articles/PMC10255001/
- Lisa Williams,At a glance: pressure injuries, 07 November 2024, https://www.britishjournalofnursing.com/content/pi-prevention/at-a-glance-pressure-injuries
- Visconti AJ, Sola OI, Raghavan PV. Pressure Injuries: Prevention, Evaluation, and Management. Am Fam Physician. 2023 Aug;108(2):166-174. PMID: 37590857.
- Padula WV, Pronovost PJ, Makic MBF, et al Value of hospital resources for effective pressure injury prevention: a cost-effectiveness analysis BMJ Quality & Safety 2019;28:132-141.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





