A sleep apnea implant is a surgically implanted device designed to keep the upper airway open during sleep. The most widely used system is the Inspire® implant, which works by stimulating the hypoglossal nerve to prevent airway collapse.
Sleep apnea is a common and potentially serious sleep disorder where breathing repeatedly stops and starts during sleep. Among its various forms, obstructive sleep apnea (OSA) is the most prevalent, caused by relaxation of throat muscles that block the airway. While traditional treatments such as Continuous Positive Airway Pressure (CPAP) machines and lifestyle changes have been mainstays of therapy, a remarkable innovation has emerged over the last decade: the sleep apnea implant.
Understanding Obstructive Sleep Apnea
Obstructive sleep apnea affects millions worldwide, disrupting sleep quality and increasing the risk of numerous health conditions, including hypertension, heart disease, stroke, diabetes, and cognitive impairment. Individuals with OSA often experience loud snoring, choking or gasping during sleep, and excessive daytime sleepiness. Diagnosis usually involves overnight sleep studies (polysomnography) to monitor breathing patterns, oxygen levels, and sleep stages.
Traditional treatments include:
- CPAP machines that deliver a steady stream of air through a mask to keep airways open.
- Oral appliances that reposition the jaw or tongue.
- Lifestyle modifications like weight loss, limiting alcohol, and sleeping on one’s side.
- Surgical interventions to remove tissue or correct anatomical abnormalities.
However, many patients find CPAP uncomfortable or intolerable, and other treatments may not provide sufficient relief. It is in this context that sleep apnea implants have gained attention.
What is a Sleep Apnea Implant?
A sleep apnea implant is a medical device surgically placed inside the body to prevent airway collapse during sleep. The most widely known and used device is the hypoglossal nerve stimulator (HNS), often referred to by the brand name Inspire.
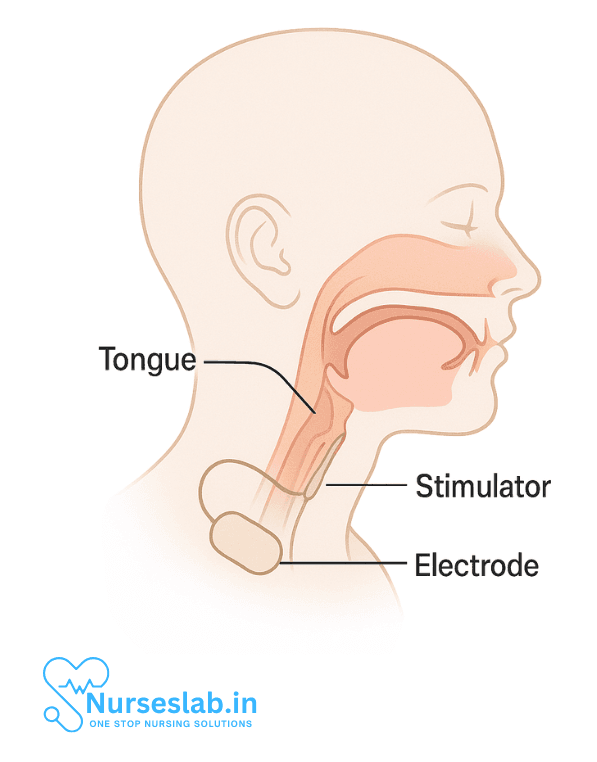
The hypoglossal nerve stimulates the muscles of the tongue. In OSA, the tongue and soft tissues relax and obstruct the airway. By stimulating the hypoglossal nerve, the implant keeps the airway open by gently moving the tongue forward during each breath.
How Does It Work?
The typical sleep apnea implant system consists of three main components:
- A small generator (similar to a pacemaker) implanted in the chest.
- A breathing sensor lead placed in the chest to detect natural breathing patterns.
- A stimulation lead that delivers mild electrical pulses to the hypoglossal nerve, activating tongue muscles.
The system is programmed and controlled via a remote. Before bedtime, the patient uses the remote to activate the device. As the patient sleeps, the sensor monitors breathing, and the stimulator sends synchronized pulses to keep the airway open. In the morning, the device is turned off with the remote, and the patient resumes normal function.
Benefits of Sleep Apnea Implants
Studies have shown that hypoglossal nerve stimulation can significantly reduce the severity of obstructive sleep apnea. Key benefits include:
- Reduced apnea episodes: Substantial decrease in the number and duration of breathing interruptions.
- Improved sleep quality: Patients report feeling more rested, with fewer arousals during the night.
- Daytime alertness: Marked improvements in concentration, mood, and energy levels.
- No external masks or hoses: Unlike CPAP, the implant is completely internal, improving comfort and compliance.
- Customizable therapy: Device settings can be tailored for individual needs and adjusted over time.
Who is a Candidate?
Not every patient with sleep apnea is eligible for an implant. The ideal candidate typically meets the following criteria:
- Diagnosed with moderate to severe obstructive sleep apnea (OSA) through a sleep study.
- Unable to tolerate or benefit sufficiently from CPAP therapy.
- Not significantly overweight (body mass index, BMI, usually less than 32 or 35, depending on guidelines).
- No complete concentric collapse of the airway at the level of the soft palate, confirmed by a special endoscopic exam during sedation (drug-induced sleep endoscopy).
- No significant medical conditions that would preclude surgery.
A thorough evaluation by a sleep specialist and ENT (ear, nose, and throat) surgeon is necessary to determine eligibility.
The Surgical Procedure
Implantation of a hypoglossal nerve stimulator is typically performed under general anesthesia and takes about two to three hours. The procedure involves:
- Making small incisions in the upper chest and under the chin.
- Placing the pulse generator in a pocket beneath the skin in the chest.
- Positioning the breathing sensor lead in the chest to detect respiratory effort.
- Locating and attaching the stimulation lead to the hypoglossal nerve beneath the jaw.
Patients usually go home the same day or after an overnight stay. After a healing period of a few weeks, the device is activated and programmed.
Recovery and Follow-up
Post-surgical recovery is typically straightforward, with mild discomfort at the incision sites. Patients are advised to avoid strenuous activities for a short period. Once the device is activated (usually 1-2 months after surgery), initial settings are fine-tuned during a sleep study.
Regular follow-up visits are important to ensure the device operates optimally and to make any necessary adjustments.
Effectiveness and Evidence
Numerous clinical trials and real-world studies have demonstrated the safety and efficacy of sleep apnea implants. Results indicate:
- Significant reduction in apnea-hypopnea index (AHI), the main measure of sleep apnea severity.
- Improvement in oxygen saturation during sleep.
- Enhanced quality of life, as measured by sleepiness and mood questionnaires.
- High rates of patient satisfaction and long-term adherence.
Most patients experience sustained benefits for years after implantation. However, like any medical device, effectiveness may vary and periodic adjustments may be required.
Risks and Considerations
As with any surgery, there are risks associated with implantation, including:
- Infection at the incision or device site.
- Pain or discomfort at the implant location.
- Swelling, bruising, or nerve injury (rare).
- Device malfunction, requiring reprogramming, repair, or replacement.
- Changes in tongue or throat sensation.
A small subset of patients may not respond as well as expected, or may develop complications requiring removal of the device.
Living With a Sleep Apnea Implant
Most recipients adapt well to their implant and report a positive impact on daily life. The device is not visible from the outside, and there are no restrictions on most activities. However, patients should inform medical providers (especially before undergoing MRI scans or surgery) about their implant.
Battery life of the pulse generator typically ranges from 7 to 10 years, after which replacement is needed through a minor procedure.
Nursing Care for Patients with Sleep Apnea Implant
Nursing care for patients with sleep apnea implants requires a multifaceted approach that encompasses patient education, perioperative and postoperative support, monitoring for complications, and long-term care management.
Preoperative Nursing Considerations
Nurses play a vital role in preparing patients for sleep apnea implant surgery. Key activities include:
- Assessment and Screening: Review patient’s history of sleep apnea, attempts at CPAP/BiPAP, and eligibility for implant.
- Education: Teach the patient about the procedure, device use, risks, benefits, and expected outcomes.
- Preparation: Ensure patients are fasting as per protocol prior to anesthesia. Confirm allergies and reconcile medications.
- Psychosocial Support: Address anxieties about surgery and living with an implant; offer counseling or support group information.
- Informed Consent: Verify that the patient understands the procedure and has signed all necessary consent forms.
Immediate Postoperative Care
After implant placement, nursing focuses on monitoring, pain control, and prevention of complications.
Monitoring and Assessment
- Vital Signs: Monitor blood pressure, pulse, respiratory rate, and oxygen saturation per protocol.
- Wound and Device Site: Inspect for redness, swelling, drainage, hematoma, or signs of infection at the incision sites.
- Pain Management: Administer prescribed analgesics and assess pain regularly. Use adjunctive comfort measures.
- Airway Assessment: Watch for airway obstruction, especially in the first hours post-surgery. Be prepared for airway support if necessary.
- Neurological Assessment: Evaluate for facial weakness, abnormal tongue movement, or speech changes, which may indicate nerve involvement.
Patient Education
- Activity Restrictions: Advise rest and avoidance of strenuous activity for the immediate postoperative period.
- Incision Care: Teach proper wound care, signs of infection, and when to call the provider.
- Device Activation: Reinforce that the device will be activated at the clinic several weeks after surgery; it is not used immediately post-op.
Long-Term Nursing Care and Follow-Up
Ongoing care for patients with sleep apnea implants involves routine monitoring, care coordination, and patient empowerment.
Device Management and Troubleshooting
- Device Activation and Adjustment: The sleep apnea implant is typically activated 4-6 weeks after surgery. Nurses should educate patients about follow-up visits for device programming and titration.
- Remote Use: Teach patients how to use the handheld remote to activate the device nightly and deactivate it each morning.
- Troubleshooting: Instruct patients on what to do if the device fails to activate, if there are unusual sensations, or if sleep quality declines.
Monitoring for Complications
- Infection: Look for fever, increasing pain, or drainage from incision sites.
- Device Malfunction: Monitor for ineffective stimulation (persistent sleep apnea symptoms) or over-stimulation (tongue twitching, discomfort).
- Nerve Injury: Assess for persistent numbness, speech difficulty, or impaired swallowing.
- Psychological Impact: Support patients adjusting to nightly device use and potential sleep disturbance during titration.
Sleep Quality and Symptom Management
- Sleep Diary: Encourage patients to keep a sleep diary noting usage, sleep duration, quality, and any side effects.
- Symptom Review: At each follow-up, ask about snoring, daytime sleepiness, cognitive function, and mood.
- Polysomnography: Some patients may require follow-up sleep studies to assess device effectiveness and adjust settings.
Patient Education and Lifelong Learning
Patient education is a cornerstone of successful implant therapy.
- How the Device Works: Use diagrams, videos, and hands-on practice to show the patient and family how the implant functions.
- Daily Routine: Reinforce nightly activation, general sleep hygiene, and device deactivation upon waking.
- When to Seek Help: List specific symptoms (e.g., high fever, severe pain, inability to swallow or speak, failure of device activation) that warrant immediate provider contact.
- Traveling with the Device: Advise on airport security, carrying a device card, and packing backup equipment.
- Lifestyle Modifications: Discuss weight management, avoidance of alcohol or sedatives, and regular exercise to maximize implant success.
Interprofessional Collaboration
Effective care requires collaboration between nurses, sleep specialists, ENT surgeons, respiratory therapists, and primary care providers.
- Care Coordination: Nurses facilitate communication among the team, schedule follow-up appointments, and relay changes in patient status.
- Patient Advocacy: Empower patients to voice concerns, participate in decision-making, and access sleep support resources.
Special Considerations for Elderly and High-Risk Patients
- Comorbidities: Adjust care plans for patients with diabetes, heart disease, or limited mobility.
- Cognitive Impairment: Provide tailored education for patients with memory loss, and involve family or caregivers in device management.
- Medication Reconciliation: Carefully monitor for drug interactions and polypharmacy risks.
Documentation and Quality Improvement
Nurses should document all care activities, patient responses, educational interventions, and device issues. Participation in quality improvement initiatives, such as data collection on sleep outcomes and complication rates, enhances care delivery.
REFERENCES
- American Thoracic Society. Upper Airway Stimulation/Hypoglossal Nerve Stimulator. https://www.thoracic.org/patients/patient-resources/resources/upper-airway-stimulation.pdf. Last reviewed 2020.
- Magaña LC, et al. (2023). Long-term generator replacement experience in hypoglossal nerve stimulator therapy recipients with CPAP-intolerant obstructive sleep apnea.
https://pubmed.ncbi.nlm.nih.gov/37003598/ - Cooper T, Sufyan AS, Aboubakr S. Hypoglossal Stimulation Device. https://www.ncbi.nlm.nih.gov/books/NBK594264/. 2023 Jul 8. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-.
- Baptista PM, et al. (2020). Hypoglossal nerve stimulation in the treatment of obstructive sleep apnea: Patient selection and new perspectives.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7026121/ - Mashaqi S, Patel SI, Combs D, et al. The Hypoglossal Nerve Stimulation as a Novel Therapy for Treating Obstructive Sleep Apnea-A Literature Review. https://pubmed.ncbi.nlm.nih.gov/33572156/. Int J Environ Res Public Health. 2021 Feb;18(4):1642.
- Sawunyavisuth B, et al. (2021). Any effective intervention to improve CPAP adherence in children with obstructive sleep apnea: A systematic review.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8165832/ - Sleep Foundation (U.S.). Hypoglossal Nerve Stimulation. https://www.sleepfoundation.org/sleep-apnea/treatment/hypoglossal-nerve-stimulation. Last updated 12/22/2023.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





