Retained products of conception (RPOC) is a term used in obstetrics and gynecology to describe the presence of placental or fetal tissue remaining in the uterus following a pregnancy event, such as miscarriage, abortion, or delivery. This condition carries significant implications for a patient’s health and well-being, necessitating timely recognition and management to prevent complications.
Definition
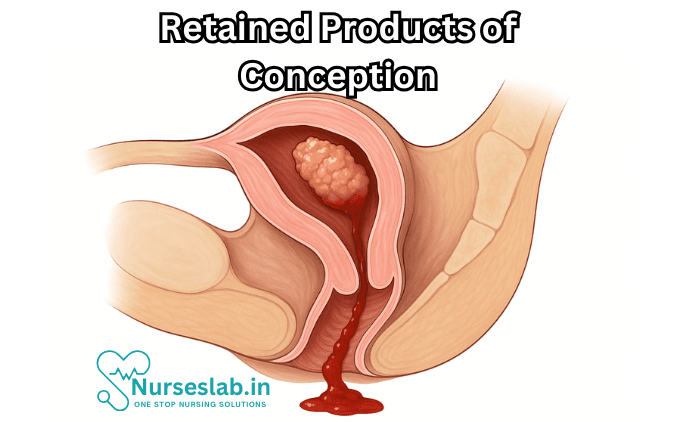
Retained products of conception refer to the persistence of placental, fetal, or other pregnancy-related tissues within the uterine cavity after the expulsion or removal of the fetus or embryo. RPOC may arise after spontaneous abortion (miscarriage), induced abortion (medical or surgical), or delivery (vaginal or cesarean). The retained tissue can range from small fragments of membranes to significant portions of placenta or fetal parts.
Etiology and Risk Factors
RPOC may occur for a variety of reasons. These include incomplete expulsion of the placenta during the third stage of labor, incomplete abortion, or inadequate evacuation during surgical or medical management of miscarriage or termination. Risk factors include:
- Early gestational age at the time of miscarriage or abortion
- Preterm delivery
- Multiple pregnancies (twins, triplets, etc.)
- Placental abnormalities (placenta accreta, increta, percreta)
- Previous history of RPOC
- Manual removal of placenta
- Infection or uterine atony during delivery
Clinical Presentation
The symptoms of RPOC can vary depending on the amount and type of tissue retained, the time elapsed since the pregnancy event, and the presence of infection or other complications. Common clinical features include:
- Abnormal vaginal bleeding (persistent or heavy bleeding post-partum or post-abortion)
- Pelvic pain or cramping
- Fever or signs of infection (endometritis, sepsis)
- Delayed return of menstruation
- Enlarged, tender uterus on examination
- Passage of tissue per vaginam
In some cases, RPOC may be asymptomatic and discovered incidentally during follow-up imaging.
Diagnosis
Early and accurate diagnosis is essential in preventing morbidity associated with RPOC. The diagnostic approach typically includes a combination of clinical assessment, laboratory evaluation, and imaging.
Clinical Assessment
A thorough history and physical examination are crucial. Key points to elicit include the timing and nature of the recent pregnancy event, the onset and pattern of symptoms, and any interventions (medical or surgical) performed.
Laboratory Evaluation
Laboratory tests may include:
- Complete blood count (CBC) – to assess for anemia and infection
- Serum beta-hCG – may remain elevated if trophoblastic tissue is retained
- Blood cultures – if there is suspicion of sepsis
Imaging
Transvaginal or transabdominal pelvic ultrasound is the imaging modality of choice for suspected RPOC. Findings that suggest retained tissue include:
- Thickened endometrial stripe (greater than 10-15mm post-partum is often considered abnormal, though cutoffs vary)
- Presence of echogenic material within the uterine cavity, sometimes with vascularity on Doppler imaging
- Irregular or heterogeneous intrauterine mass
However, ultrasound findings should always be interpreted in conjunction with clinical symptoms, as normal postpartum changes can mimic or obscure RPOC.
Management
The management of RPOC depends on the size and type of retained tissue, patient symptoms, and risk of complications.
Expectant Management
In select cases, especially when the retained tissue burden is small and the patient is stable with mild symptoms, expectant management may be considered. This involves careful monitoring for spontaneous expulsion of tissue, with follow-up imaging and clinical assessment.
Medical Management
Medical therapy may include the administration of uterotonic agents such as misoprostol, which induces uterine contractions to help expel retained tissue. Medical management is often considered in early pregnancy loss or for patients who are not candidates for surgery.
Surgical Management
Surgical intervention is indicated in cases of significant hemorrhage, infection, hemodynamic instability, or failure of medical/expectant management. Procedures include:
- Dilation and curettage (D&C) – the most common surgical method
- Manual vacuum aspiration (MVA)
- Hysteroscopic removal – in select cases where tissue is adherent or difficult to remove
In rare or severe cases, such as when RPOC is complicated by abnormal placentation (e.g., placenta accreta), a hysterectomy may be required.
Complications
If RPOC is not identified and managed promptly, it can lead to significant complications, including:
- Severe or prolonged vaginal bleeding, potentially resulting in anemia or hypovolemic shock
- Infection (endometritis, septicemia)
- Infertility due to intrauterine adhesions (Asherman’s syndrome)
- Uterine perforation (from invasive procedures)
- Disseminated intravascular coagulation (DIC) in severe cases
Prevention
- While not all cases of RPOC can be prevented, certain measures may reduce the risk:
- Adequate training and experience of health care providers
- Careful inspection of the placenta and membranes after delivery or abortion to ensure completeness
- Use of ultrasound guidance during evacuation procedures
- Prompt intervention if postpartum hemorrhage or incomplete abortion is suspected
Nursing Care of Patients with Retained Products of Conception (RPOC)
1. Assessment and Early Identification
- Monitor Vital Signs: Regularly check temperature, pulse, blood pressure, and respiratory rate to detect early signs of shock or infection.
- Assess Vaginal Bleeding: Note the amount, colour, and presence of clots. Sudden increase in bleeding or foul-smelling discharge must be reported immediately.
- Evaluate Pain: Ask about the location, intensity, and character of abdominal pain. Increasing pain may indicate worsening condition.
- Check for Signs of Infection: Look for fever, chills, malaise, and uterine tenderness.
- History Taking: Obtain detailed obstetric and menstrual history, including the events leading up to the current situation.
2. Immediate Nursing Interventions
- Ensure Haemodynamic Stability: Initiate intravenous access if not already done. Administer fluids as per physician’s orders to prevent shock.
- Prepare for Evacuation Procedures: Assist in preparing the patient physically and emotionally for procedures like dilation and curettage (D&C) or manual vacuum aspiration, as advised by the medical team.
- Administer Medications: Give antibiotics, analgesics, or uterotonics as prescribed. Monitor for adverse reactions.
- Maintain Aseptic Technique: Prevent infection during all invasive procedures and dressing changes.
3. Ongoing Monitoring and Support
- Monitor Output: Record urine output and ensure adequate hydration.
- Observe for Complications: Watch for signs of heavy bleeding, hypotension, tachycardia, or signs of sepsis.
- Emotional Support: Provide psychological support, acknowledging the emotional impact of pregnancy loss or complications. Offer privacy and empathetic listening.
- Family Involvement: Involve family members in care, explaining the situation and procedures as appropriate, in culturally sensitive language.
4. Patient Education
- Discharge Instructions: Educate the patient on signs of complications that require immediate medical attention, such as heavy bleeding, severe pain, or fever.
- Hygiene and Self-care: Advise on proper perineal hygiene to prevent infection.
- Follow-up Care: Stress the importance of follow-up visits for ultrasound or clinical assessment to ensure complete evacuation.
- Family Planning: Counsel on contraceptive options and spacing of future pregnancies, as per the patient’s needs and preferences.
5. Documentation
- Document all findings, interventions, patient responses, and communications with the healthcare team in detail.
- Record the amount and nature of vaginal bleeding, pain scores, administered medications, and vital sign trends.
6. Cultural and Ethical Considerations
- Respect cultural beliefs and practices related to pregnancy and miscarriage.
- Maintain confidentiality and dignity of the patient at all times.
- Be sensitive to the emotional and psychological needs of the patient and her family, especially in the context of societal expectations around fertility and childbirth in India.
REFERENCES
- American Pregnancy Association. Retained Placenta. https://americanpregnancy.org/healthy-pregnancy/labor-and-birth/retained-placenta/. Modified 6/1/2023.
- Chawla S, Sharma R. Retained Products of Conception (RPOC): Diagnosis, Complication & Management. https://pubmed.ncbi.nlm.nih.gov/37916054/. J Obstet Gynaecol India. 2023 Oct;73(5):374-380. .
- Foreste V, Gallo A, Manzi A, Riccardi C, Carugno J, Sardo ADS. Hysteroscopy and Retained Products of Conception: An Update. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8613498/. Gynecol Minim Invasive Ther. 2021 Oct-Dec;10(4):203-209. Publish 2021 Nov 5.
- Hamel CC, van Wessel S, Carnegy A, et al. Diagnostic criteria for retained products of conception-A scoping review. https://pubmed.ncbi.nlm.nih.gov/34244998/. Acta Obstet Gynecol Scand. 2021 Dec;100(12):2135-2143.
- Perlman NC, Carusi DA. Retained placenta after vaginal delivery: risk factors and management. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6789409/. Int J Womens Health. 2019 Oct;11:527-534. Published 2019 Oct 7.
- Schulte RL, Fox R, Anderson J, et al. Medical management of retained products of conception: A prospective observational study. https://pubmed.ncbi.nlm.nih.gov/37120911/. Eur J Obstet Gynecol Reprod Biol. 2023 Jun;285:153-158.
- Tzur Y, Berkovitz-Shperling R, Goitein Inbar T, et al. Expectant vs medical management for retained products of conception after medical termination of pregnancy: a randomized controlled study. https://pubmed.ncbi.nlm.nih.gov/35752301/. Am J Obstet Gynecol. 2022 Oct;227(4):599.e1-599.e9. .
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





