A colonoscopy Procedure is a diagnostic and screening procedure that uses a flexible scope to examine the colon for polyps, bleeding, inflammation, and early signs of colorectal cancer. It supports prevention, early detection, and effective treatment planning
Introduction
Colonoscopy is a vital medical procedure that has become a cornerstone in the diagnosis and prevention of diseases affecting the large intestine (colon) and rectum. Over the past few decades, it has helped detect numerous conditions at their earliest stages, significantly improving patient outcomes. For many, the thought of undergoing a colonoscopy can be daunting, often due to a lack of clear information or a fear of the unknown.
Purpose and Indications
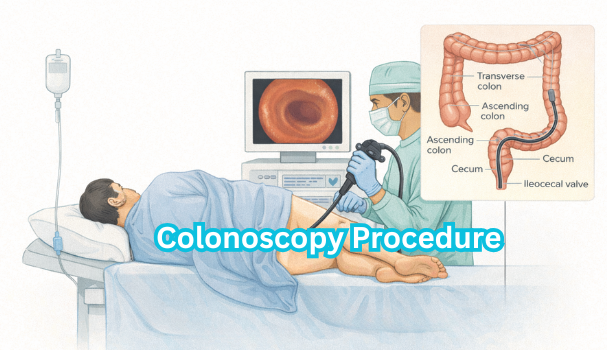
A colonoscopy is performed primarily to examine the inner lining of the colon and rectum using a flexible, tube-like instrument called a colonoscope. The primary purpose is to detect abnormalities such as polyps, inflammation, ulcers, tumours, and sources of bleeding. Colonoscopy is not only diagnostic but can also be therapeutic, allowing doctors to remove polyps or take tissue samples (biopsies) during the same procedure.
Common Reasons for Colonoscopy
- Screening for Colorectal Cancer: Colonoscopy is the gold standard for colorectal cancer screening, especially for those aged 45 and above, or earlier for individuals with a family history of the disease.
- Investigating Digestive Symptoms: Chronic diarrhoea, constipation, unexplained weight loss, abdominal pain, or rectal bleeding may prompt a doctor to recommend a colonoscopy.
- Monitoring Inflammatory Bowel Disease (IBD): Patients with conditions like ulcerative colitis or Crohn’s disease often require regular colonoscopies to monitor disease progression and check for complications.
- Polyp Surveillance: Individuals who have previously had colon polyps removed may need periodic colonoscopies to ensure no new growths have developed.
- Evaluating Anaemia: If there is unexplained iron-deficiency anaemia, especially in older adults, colonoscopy helps rule out bleeding sources in the colon.
Preparation for Colonoscopy
Proper preparation is crucial for the success and safety of a colonoscopy. A clean colon allows doctors to have a clear view and reduces the risk of missing important findings.
Dietary Restrictions
- Low-Residue Diet: A few days before the procedure, patients are usually advised to switch to a low-fibre or low-residue diet. This includes avoiding whole grains, seeds, nuts, raw fruits, and vegetables.
- Clear Liquid Diet: On the day before the colonoscopy, only clear liquids such as water, coconut water, clear soups, black tea, and clear juices are allowed. Coloured drinks (especially red or purple) should be avoided as they can be mistaken for blood during the test.
Bowel Preparation
- Laxatives: Patients are given a special laxative solution, usually in split doses, to drink as per doctor’s instructions. This induces diarrhoea and cleanses the bowel.
- Hydration: It is important to drink plenty of clear fluids to prevent dehydration during the preparation process.
Patient Instructions
- Medication Adjustments: Some medications, especially blood thinners, diabetes medicines, and iron supplements, may need to be adjusted or temporarily stopped. Always consult your doctor before making any changes.
- Arrangements for the Day: As sedation is commonly used, patients should arrange for a responsible adult to accompany them home after the procedure.
- Clothing and Personal Items: Wear comfortable, loose-fitting clothes and leave valuables at home on the day of the test.
Colonoscopy Procedure Steps
Understanding the step-by-step process can help reduce anxiety and ensure a smoother experience.
Equipment Used
- Colonoscope: A long, flexible tube about the thickness of a finger, equipped with a light, camera, and channels for instruments.
- Monitors: High-definition monitors display real-time images from the colonoscope, allowing the doctor to guide the instrument and record findings.
- Accessories: Special tools can be passed through the colonoscope to take biopsies, remove polyps, or manage bleeding.
Sedation and Positioning
- Sedation: Most patients receive mild to moderate sedation (conscious sedation) to help them relax and minimise discomfort. Some centres offer deeper sedation or general anaesthesia, depending on the patient’s needs and the centre’s protocols.
- Positioning: The patient usually lies on their left side with knees drawn up towards the chest. This position helps straighten the colon for easier scope passage.
Step-by-Step Process
- Initial Assessment: Vital signs are checked, and the sedation is administered. The procedure is explained again, and any last-minute questions are answered.
- Scope Insertion: The lubricated colonoscope is gently inserted into the rectum and slowly advanced through the entire colon. Air or carbon dioxide is insufflated to expand the colon and improve visibility.
- Inspection: As the scope is advanced, the doctor carefully examines the lining for any abnormalities. The camera transmits images to the monitor for real-time assessment.
- Therapeutic Actions: If polyps or suspicious areas are found, they can be removed or biopsied during the same procedure using tiny instruments passed through the colonoscope.
- Withdrawal and Final Check: The scope is slowly withdrawn, and the doctor continues to inspect the colon lining thoroughly on the way out, as some abnormalities are more visible during withdrawal.
- Completion: The procedure usually lasts between 20 and 45 minutes, depending on the findings and complexity.
Risks and Benefits
Like all medical procedures, colonoscopy has both risks and benefits. However, it is generally considered a safe and highly effective diagnostic tool.
Benefits of Colonoscopy
- Early Detection: Colonoscopy can detect precancerous polyps and early-stage cancers, allowing for timely treatment and significantly improving survival rates.
- Prevention: Removing polyps during colonoscopy can prevent the development of colorectal cancer.
- Comprehensive Evaluation: It allows direct visualisation of the entire colon, making it more accurate than other tests such as barium enema or CT colonography.
- Therapeutic Capability: Besides diagnosis, colonoscopy enables treatment of certain conditions during the same session, such as polyp removal and control of bleeding.
Potential Risks and Complications
- Bleeding: Minor bleeding can occur, especially after polyp removal or biopsy. It is usually self-limiting but may require additional treatment in rare cases.
- Perforation: There is a very small risk (less than 1 in 1,000 procedures) of creating a hole in the colon wall, which may require surgical repair.
- Adverse Reaction to Sedation: Some patients may experience side effects such as nausea, vomiting, or allergic reactions to the sedative medications.
- Infection: The risk of infection is extremely low, as the instruments are thoroughly sterilised.
- Incomplete Examination: In rare instances, technical difficulties or poor bowel preparation may prevent complete visualisation of the colon, necessitating a repeat procedure.
It is important to remember that the benefits of early detection and prevention far outweigh the minimal risks associated with colonoscopy for most patients.
Post-Procedure Care
After the colonoscopy, most patients recover quickly and can resume their normal activities within a day or two. However, certain precautions and care measures are advised.
Recovery Process
- Observation: Patients are monitored in a recovery area until the effects of sedation wear off, typically for 30 to 60 minutes.
- Diet: Once awake and alert, patients can usually start with light meals. Some may experience mild bloating, cramping, or gas, which usually resolves within a few hours.
- Rest: It is recommended to rest for the remainder of the day and avoid driving, operating machinery, or making important decisions due to the lingering effects of sedation.
- Follow-Up Instructions: The doctor will provide specific advice regarding resuming medications, dietary restrictions, and signs to watch out for.
Managing Side Effects
- Minor Discomfort: Mild abdominal discomfort, bloating, or a feeling of fullness is common and usually temporary.
- Bleeding: A small amount of blood with the first bowel movement after polyp removal is not unusual. However, persistent or heavy bleeding should be reported to the doctor immediately.
- Signs of Complications: Severe abdominal pain, fever, chills, or persistent vomiting are rare but may indicate complications. Seek medical attention promptly if these occur.
Follow-Up Care
- Test Results: If biopsies were taken or polyps removed, results are usually available within a week. The doctor will discuss the findings and recommend further steps if needed.
- Repeat Colonoscopy: Depending on the findings, follow-up colonoscopies may be scheduled at intervals ranging from 1 to 10 years.
Recent Advancements in Colonoscopy
Medical technology is constantly evolving, and colonoscopy has seen significant advancements in recent years, making the procedure safer, more comfortable, and more accurate.
Enhanced Visualisation
- High-Definition Scopes: Modern colonoscopes provide clearer, more detailed images, allowing for better detection of small polyps and subtle abnormalities.
- Narrow Band Imaging (NBI): This technology uses special light filters to enhance the visibility of blood vessels and surface patterns, aiding in the identification of abnormal tissue.
Improved Comfort and Safety
- Carbon Dioxide Insufflation: Using carbon dioxide instead of air to expand the colon reduces post-procedure bloating and discomfort, as it is absorbed by the body more quickly.
- Water Immersion Techniques: Some centres now use water instead of air to help advance the scope, which can make the procedure more comfortable and improve visibility.
Artificial Intelligence (AI) Integration
- Computer-Aided Detection: AI-powered systems can assist doctors in identifying polyps and other abnormalities, potentially increasing the detection rate and reducing the chance of missed lesions.
Capsule Endoscopy
- Non-Invasive Option: For some patients, a capsule containing a tiny camera can be swallowed to take images of the digestive tract. While not a replacement for colonoscopy, it offers a less invasive alternative for certain cases.
Patient-Centred Improvements
- Personalised Preparation: Newer bowel preparation regimens are being developed to improve tolerability and effectiveness, reducing the discomfort associated with traditional methods.
- Remote Consultations: Telemedicine options are helping patients understand the procedure and receive pre- and post-procedure counselling from the comfort of their homes.
Nursing Care for Patients Undergoing Colonoscopy Procedure
As a nurse, providing care to patients undergoing colonoscopy involves a multifaceted approach, encompassing pre-procedure preparation, intra-procedure assistance, and post-procedure care
Pre-Procedure Nursing Care
Pre-procedure care is crucial to ensure the patient is adequately prepared, both physically and psychologically, for the colonoscopy. This phase includes patient assessment, education, bowel preparation, and addressing any anxieties or concerns.
1. Patient Assessment
- Medical History: Review the patient’s medical history, including previous colonoscopies, gastrointestinal disorders, allergies (especially to medications or latex), and current medications (notably anticoagulants, antiplatelets, or diabetic medications).
- Physical Assessment: Assess vital signs, hydration status, and overall health. Identify any contraindications to the procedure, such as acute diverticulitis or suspected perforation.
- Consent: Ensure that informed consent has been obtained and documented, with the patient understanding the risks, benefits, and alternatives.
2. Patient Education
- Explain the purpose, steps, and expected sensations during the colonoscopy.
- Discuss the importance and details of bowel preparation, dietary restrictions (usually a clear liquid diet 24 hours prior), and fasting requirements.
- Provide written and verbal instructions to reinforce understanding.
- Address questions and alleviate fears about discomfort, embarrassment, or outcomes.
3. Bowel Preparation
- Administer prescribed bowel-cleansing agents, such as polyethylene glycol or sodium picosulphate, as per protocol.
- Monitor the patient for side effects like nausea, vomiting, dehydration, or electrolyte imbalance.
- Encourage fluid intake as allowed to prevent dehydration.
- Assess the effectiveness of bowel preparation by evaluating stool output; the bowel should be clear of solid matter.
4. Medication Management
- Review and clarify instructions regarding temporary discontinuation of certain medications, particularly anticoagulants and antiplatelets, in consultation with the medical team.
- Ensure diabetic patients receive specific guidance about insulin or oral hypoglycaemic agents due to fasting requirements.
5. Intra-Procedure Nursing Care
During the colonoscopy, the nurse plays a critical role in patient monitoring, comfort, and procedural support. Key responsibilities include:
- Patient Identification and Verification: Confirm the patient’s identity, procedure, and consent before commencement.
- Monitoring: Continuously monitor vital signs (heart rate, blood pressure, oxygen saturation, respiratory rate), level of consciousness, and comfort, especially if sedation is used.
- Assistance: Assist the endoscopist by positioning the patient (usually left lateral position), passing instruments, and managing biopsy samples or polypectomy snares.
- Airway Management: Be vigilant for signs of respiratory depression or aspiration, particularly in sedated patients.
- Reassurance: Provide ongoing verbal reassurance, explaining what is happening as appropriate and addressing any discomfort or anxiety.
- Documentation: Record procedural details, medications administered (including dosage and time), patient responses, and any complications.
Post-Procedure Nursing Care
After the colonoscopy, patients require observation and support to recover from sedation and to monitor for complications. The nurse’s responsibilities include:
1. Recovery and Monitoring
- Observation: Monitor vital signs, level of consciousness, and respiratory status until the patient is fully alert and stable.
- Assessment: Check for abdominal pain, distension, rectal bleeding, or signs of perforation (e.g., severe pain, tachycardia, hypotension).
- Hydration and Nutrition: Once fully conscious, offer fluids and light food as tolerated, unless otherwise instructed.
- Mobility: Assist the patient with ambulation as they may be unsteady due to residual sedation.
2. Patient Education and Discharge Planning
- Provide written and verbal instructions on post-procedure care, including signs and symptoms of complications (e.g., persistent bleeding, severe pain, fever) and when to seek medical attention.
- Advise on resumption of regular diet and medications, based on the endoscopist’s recommendations.
- Discuss when normal activities, including driving, can be resumed (usually not for 24 hours if sedation was used).
- Arrange for a responsible adult to accompany the patient home if sedation was administered.
Managing Potential Complications
Although colonoscopy is generally safe, nurses must be vigilant for possible complications, which include:
- Perforation: A rare but serious complication presenting with severe abdominal pain, tenderness, and sometimes signs of shock. Immediate medical attention is required.
- Bleeding: Most commonly occurs after polypectomy. Monitor for rectal bleeding, which may be immediate or delayed.
- Adverse Reactions to Sedation: Watch for respiratory depression, hypotension, or allergic reactions.
- Infection: Uncommon, but possible if biopsies are taken or perforation occurs.
- Dehydration and Electrolyte Imbalance: May result from bowel preparation, especially in vulnerable patients.
Psychological Support and Patient Centred Care
Undergoing a colonoscopy can be a source of anxiety, embarrassment, and discomfort for many patients. Nurses have a unique opportunity to provide psychological support by:
- Listening empathetically to concerns and fears.
- Maintaining patient dignity and privacy at all times.
- Using clear, jargon-free language.
- Encouraging questions and participation in care decisions.
- Being sensitive to cultural, religious, and personal preferences.
Special Considerations
- Elderly Patients: May be at increased risk of complications such as dehydration, electrolyte disturbances, or sedation-related issues. Adjust care accordingly and involve family or carers as needed.
- Paediatric Patients: Require age-appropriate explanations and reassurance. Parental involvement is essential.
- Patients with Disabilities or Communication Difficulties: Adapt communication strategies and involve support persons or interpreters if necessary.
Documentation and Legal Considerations
- Accurately document all aspects of care, including assessments, interventions, patient responses, and any incidents or complications.
- Ensure all legal and organisational protocols are followed, particularly regarding consent and medication administration.
REFERENCES
- American Society for Gastrointestinal Endoscopy. Understanding Colonoscopy. https://www.asge.org/home/for-patients/patient-information/understanding-colonoscopy.
- Screening for colorectal cancer: U.S. Preventive Services Task Force Recommendation Statement. Journal of the American Medical Association. 2021; doi:10.1001/jama.2021.6238.
- American Society of Anesthesiologists. Colonoscopy . https://www.asahq.org/madeforthismoment/preparing-for-surgery/procedures/colonoscopy/.
- Cancer.Net. Colonoscopy (https://www.cancer.net/navigating-cancer-care/diagnosing-cancer/tests-and-procedures/colonoscopy).
- Gupta S, et al. Recommendations for follow-up after colonoscopy and polypectomy: A consensus update by the U.S. Multi-Society Task Force on Colorectal Cancer. Gastroenterology. 2020; doi:10.1053/j.gastro.2019.10.026.
- Centers for Disease Control and Prevention. Colorectal Cancer Screening Tests. https://www.cdc.gov/cancer/colorectal/basic_info/screening/tests.htm.
- Kim SY, Kim HS, Park HJ. Adverse events related to colonoscopy: global trends and future challenges. World J Gastroenterol. 2019;25(2):190–204. doi:10.3748/wjg.v25.i2.190
- National Institute of Diabetes and Digestive and Kidney Diseases. Colonoscopy. https://www.niddk.nih.gov/health-information/diagnostic-tests/colonoscopy
- Shaukat A, Kahi CJ, Burke CA, Rabeneck L, Sauer BG, Rex DK. ACG clinical guidelines: Colorectal cancer screening 2021. Am J Gastroenterol. 2021;116(3):458-479.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





