A mastectomy is a surgical procedure to remove all or part of one or both breasts, typically as a treatment for breast cancer or, in some cases, as a preventative measure for individuals at high risk. The decision to undergo a mastectomy is profound and complex, combining medical considerations, personal values, and emotional factors.
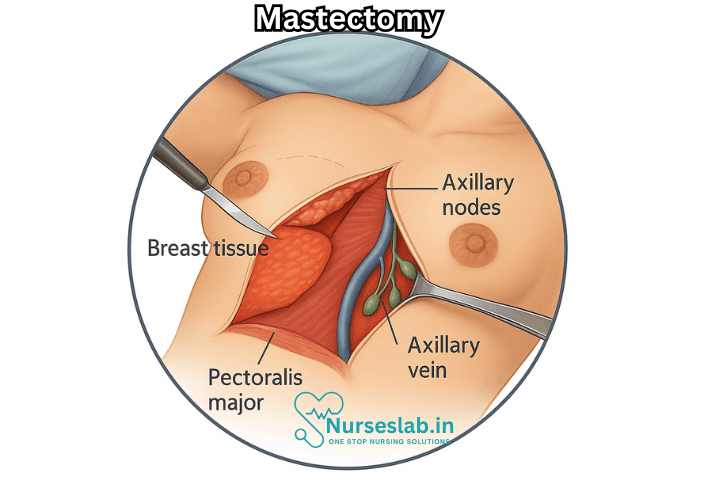
What is a Mastectomy?
A mastectomy involves the removal of breast tissue to treat or prevent disease, most commonly breast cancer. The procedure may be performed on one breast (unilateral mastectomy) or both breasts (bilateral mastectomy). For many, this surgery represents more than just a medical intervention—it is a step in their journey through cancer or a proactive effort to reduce risk.
History and Evolution of Mastectomy
The concept of surgically removing the breast dates back centuries, but the modern mastectomy evolved over the past 150 years. In the late 19th century, William Stewart Halsted introduced the radical mastectomy, which involved removing the entire breast, underlying chest muscles, and lymph nodes. While effective in removing cancer, this procedure was highly invasive and disfiguring. Over time, medical understanding advanced, and less extensive but equally effective surgeries were developed, balancing cancer control with quality of life and physical appearance.
Types of Mastectomy
There are several types of mastectomy, each tailored to the patient’s specific diagnosis, anatomy, and preferences:
- Total (Simple) Mastectomy: Removes the entire breast, including the nipple, areola, and most of the overlying skin, but does not remove lymph nodes under the arm or muscle tissue beneath the breast.
- Modified Radical Mastectomy: Removes the entire breast along with some underarm (axillary) lymph nodes. This is the most common surgery for invasive breast cancer.
- Radical Mastectomy: Involves the removal of the entire breast, axillary lymph nodes, and the chest wall muscles under the breast. It is now rarely performed, reserved for cancers that have spread to the chest muscles.
- Skin-Sparing Mastectomy: Removes the breast tissue, nipple, and areola but preserves most of the breast skin, which is beneficial for immediate reconstruction.
- Nipple-Sparing Mastectomy: Removes the breast tissue but preserves the skin, nipple, and areola. This option may be suitable for certain cancers or preventative mastectomies.
- Double (Bilateral) Mastectomy: Removal of both breasts, either as a treatment or as a preventative measure (“prophylactic mastectomy”) for those at high risk, such as carriers of BRCA1 or BRCA2 genetic mutations.
Indications for Mastectomy
A mastectomy may be recommended in various situations, such as:
- Large or multifocal tumors that cannot be effectively removed with breast-conserving surgery (lumpectomy).
- Personal preference, especially for those wishing to minimize future cancer risk.
- Genetic predisposition to breast cancer (e.g., BRCA mutations).
- Previous radiation therapy to the breast area, which limits options for repeat breast-conserving surgery.
- Inflammatory breast cancer or tumors with extensive ductal carcinoma in situ (DCIS).
- Recurrence of breast cancer after prior breast-conserving therapy.
Preparation and Procedure
Preparation for a mastectomy involves consultations with a multidisciplinary medical team, including a surgeon, medical oncologist, radiation oncologist, and, when appropriate, a plastic or reconstructive surgeon. Preoperative imaging (such as mammography, ultrasound, or MRI) is used to determine the extent of disease. Patients may be advised to stop certain medications before surgery and to arrange for help during the recovery period.
During the procedure, which typically lasts between 1 and 3 hours, patients are placed under general anesthesia. The surgeon makes an incision (the location and pattern depend on the type of mastectomy and reconstruction planned) and removes the specified tissue. If lymph nodes are to be removed, a separate incision may be made in the underarm area.
Recovery and Postoperative Care
The hospital stay after mastectomy can range from a few hours (outpatient surgery) to a couple of days, depending on the extent of the procedure and reconstruction. Wound drains may be placed to prevent fluid buildup and are typically removed within one to two weeks. Patients are given instructions on wound care, pain management, and physical activity.
Recovery time varies, but most people can resume light activities within 1–2 weeks and more strenuous activities within 4–6 weeks. Physical therapy or specific exercises may be recommended to help restore range of motion, especially if lymph nodes were removed.
Risks and Complications
Mastectomy is generally safe but, like any surgery, carries risks. Potential complications include:
- Bleeding or hematoma formation
- Infection at the surgical site
- Pain or numbness in the chest or arm
- Swelling (lymphedema) of the arm, especially when lymph nodes are removed
- Poor wound healing or scarring
- Seroma (fluid accumulation under the skin)
- Shoulder stiffness or limited range of motion
- Emotional or psychological distress
Breast Reconstruction and Alternatives
Many individuals choose to undergo breast reconstruction after mastectomy, either immediately during the same surgery or delayed until after additional cancer treatments. Reconstruction options include:
- Implant-based reconstruction: Using silicone or saline implants to restore breast shape.
- Autologous tissue reconstruction: Utilizing tissue from another part of the body (such as the abdomen or back) to create a new breast.
- Combination of both methods.
Some opt not to have reconstruction and instead use external breast prostheses or embrace a flat chest. The decision is highly personal and influenced by medical considerations, lifestyle, and psychological factors.
Alternatives to mastectomy include breast-conserving surgery (lumpectomy) followed by radiation therapy, when appropriate. The choice depends on tumor size, location, stage, and patient preference.
Emotional and Psychological Impact
A mastectomy can have profound emotional and psychological effects. Reactions may include relief, sadness, anxiety, grief over loss of a body part, or concerns about body image and sexuality. Support from mental health professionals, support groups, loved ones, and, if desired, reconstructive surgeons can help individuals navigate the emotional aftermath.
Life After Mastectomy
After a mastectomy, regular follow-up visits with healthcare providers are important to monitor healing, manage any complications, and screen for recurrence. Many people adapt well and return to their usual activities, though some experience lasting changes in sensation, appearance, or emotional state.
Advances in surgical techniques, reconstructive options, and psychological support have improved outcomes and quality of life following mastectomy. Ongoing research seeks to further reduce complications, enhance cosmetic results, and expand options for those facing breast cancer.
Nursing Care of a Patient with Mastectomy
Nursing care for post-mastectomy patients is a multi-faceted process, addressing physical, psychological, and emotional needs. The objective is to promote optimal healing, prevent complications, and support the patient’s adjustment to the changes brought by surgery.
Preoperative Nursing Care
Patient Education and Psychological Preparation
- Providing Information: Nurses play a critical role in educating patients about the nature of the surgery, its purpose, possible outcomes, and the expected postoperative course. This helps allay fears and anxiety.
- Emotional Support: Addressing the emotional impact is vital. The loss of a breast can cause anxiety, depression, body image disturbances, and fears about femininity or sexuality. Nurses should encourage patients to express their feelings and offer reassurance and resources such as counseling.
- Preoperative Instructions: Patients should be informed about pre-surgery fasting, medication restrictions, and hospital procedures. Demonstrating breathing exercises and arm exercises that will be performed postoperatively can increase compliance and reduce anxiety.
- Family Involvement: Involving family members in education and support can facilitate recovery and adjustment.
Immediate Postoperative Nursing Care
Monitoring and Assessment
- Vital Signs: Monitor vital signs frequently (temperature, pulse, respiration, blood pressure) to detect early signs of shock, hemorrhage, or infection.
- Pain Management: Assess pain regularly using an appropriate scale and administer prescribed analgesics. Encourage relaxation techniques and positioning to minimize discomfort.
- Wound Care: Inspect the surgical site for signs of bleeding, infection (redness, swelling, drainage), and dehiscence. Maintain a sterile technique during dressing changes to prevent infection.
- Drain Management: Many patients will have surgical drains (e.g., Jackson-Pratt) to prevent fluid accumulation. Nurses should monitor output, assess for blockage, and educate patients and families about drain care.
- Monitor for Lymphedema: Following lymph node removal, monitor for swelling of the arm on the affected side. Early detection and intervention can prevent complications.
Positioning and Mobility
- Arm Care: The arm on the affected side should not be used for blood pressure measurements, injections, or blood draws to prevent trauma and lymphedema.
- Positioning: Position the patient in a semi-Fowler’s (head elevated) position with the affected arm elevated on a pillow to facilitate lymphatic drainage and reduce swelling.
- Early Mobilization: Encourage movement of the fingers and hand as soon as possible. Gentle arm exercises, as taught preoperatively, should begin when allowed by the surgeon to prevent stiffness and maintain range of motion.
Preventing Complications
Infection Prevention
- Sterile Technique: Use aseptic technique for all wound and drain care. Educate the patient and family about hand hygiene and signs of infection.
- Monitor for Systemic Signs: Be vigilant for fever, chills, or malaise, which may indicate systemic infection.
Managing Lymphedema
- Education: Teach the patient to avoid trauma to the affected arm (cuts, burns, insect bites) and to wear gloves during activities like gardening or dishwashing.
- Compression Garments: Compression sleeves may be recommended to minimize swelling. Nurses should instruct on proper use and care.
- Exercise: Gentle exercises and elevation help prevent fluid buildup.
Pain and Discomfort
- Analgesics: Administer as prescribed and reassess pain frequently.
- Non-Pharmacological Methods: Encourage relaxation, guided imagery, deep breathing exercises, or cold packs if appropriate.
Prevention of Deep Vein Thrombosis (DVT)
- Mobilization: Encourage early ambulation as tolerated.
- Stockings: Apply anti-embolism stockings if prescribed.
- Monitoring: Assess for signs of DVT such as calf pain, redness, swelling, or tenderness.
Psychosocial and Emotional Support
- Body Image and Self-Esteem: Recognize the impact of mastectomy on self-image and sexuality. Offer supportive counseling and facilitate referral to support groups or peer counselors.
- Communication: Provide a safe, private environment for the patient to express concerns. Be an empathetic listener and validate their feelings.
- Involving Family: Encourage family presence and participation. Educate family members about the recovery process and ways to provide support without being overprotective.
- Rehabilitation: Support the patient’s gradual return to normal activities and participation in decision-making regarding prosthetics or reconstructive surgery.
Patient Education and Discharge Planning
Home Care Instructions
- Wound and Drain Care: Teach the patient and family how to care for the incision and drains, recognize signs of infection, and manage dressings.
- Pain Management: Instruct on prescribed analgesics, when to take them, and when to seek help for uncontrolled pain.
- Arm Care: Remind about precautions such as avoiding blood draws, blood pressure, or injections on the affected side, and protecting the arm from injury.
- Activity Guidelines: Encourage gradual return to normal activities, avoiding heavy lifting or strenuous exercise until cleared by the physician.
- Lymphedema Prevention: Explain the importance of exercises and elevation, the use of compression sleeves if prescribed, and monitoring for swelling.
- Follow-Up: Stress the importance of attending all follow-up appointments for wound checks, pathology results, and ongoing care.
- Emotional Support: Provide contact information for counseling services, support groups, and educational resources.
Prosthetics and Reconstructive Surgery
- Options: Discuss options for breast prostheses or reconstructive surgery if the patient is interested. Provide information on the timing, risks, and benefits.
- Fitting and Use: Arrange for a professional fitting of a prosthesis and instruct on care and maintenance.
Sexuality and Intimacy
- Open Discussion: Encourage open conversations about changes in body image, intimacy concerns, and fears about sexual relationships.
- Support: Offer resources such as counseling or support groups specializing in sexuality after cancer treatment.
Long-Term Care and Rehabilitation
Ongoing Monitoring
- Surveillance: Regular follow-up is essential to monitor for recurrence or complications.
- Screening: Advise on routine screening for breast cancer if unilateral mastectomy was performed.
Physical Rehabilitation
- Physical Therapy: Referral to a physiotherapist for tailored exercise programs can restore strength and mobility.
- Occupational Therapy: May be needed to assist with adapting to new functional limitations.
Psychological Support
- Counseling: Continued access to psychological counseling or support groups can help patients adjust emotionally.
- Peer Support: Contact with others who have undergone similar experiences offers valuable reassurance and advice.
Special Considerations
Care of Elderly Patients
- Individualized Approach: Elderly patients may need more assistance with mobility, wound care, and home adaptations.
- Polypharmacy: Monitor for drug interactions and complications due to multiple medications.
Cultural Sensitivity
- Respect Beliefs: Nurses should be aware of and respect cultural beliefs and practices regarding body image, illness, and healing.
- Language Barriers: Provide interpreter services as needed to ensure understanding and adherence to care plans.
REFERENCES
- BreastCancer.org. Mastectomy vs. Lumpectomy. https://www.breastcancer.org/treatment/surgery/mastectomy-vs-lumpectomy. Updated 12/19/2023.
- Cancer Research UK. Surgery to remove your breast (mastectomy) (https://www.cancerresearchuk.org/about-cancer/breast-cancer/treatment/surgery/remove-whole-breast-mastectomy). Updated 1/8/2024.
- Townsend CM Jr., et al. Diseases of the breast. In: Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice. 21st ed. Elsevier; 2022. https://www.clinicalkey.com.
- Goethals A, Rose J. Mastectomy. https://www.ncbi.nlm.nih.gov/books/NBK538212/). [Updated 2022 May 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Updated 10/6/2022.
- National Breast Cancer Foundation (U.S.). Recovery. https://www.nationalbreastcancer.org/blog/checklist-for-recovery-aftermastectomy/#:~:text=Mastectomy%20recovery%20can%20take%20anywhere,often%20closer%20to%204%20weeks). Updated 5/14/2024.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





