Ketogenesis is the biochemical process in the liver that produces ketone bodies—acetoacetate, β-hydroxybutyrate, and acetone—from fatty acids. It supplies energy to the brain, muscles, and heart during fasting, prolonged exercise, or carbohydrate restriction.
Introduction
Ketogenesis, the process by which the body produces ketone bodies, is particularly relevant in contexts such as diabetes, starvation, and metabolic disorders. One of the most significant metabolic processes relevant to nursing is ketogenesis—a pathway that not only reflects the body’s adaptation to energy shortages but also plays a pivotal role in several clinical scenarios.
Basics of Ketogenesis
Definition of Ketogenesis
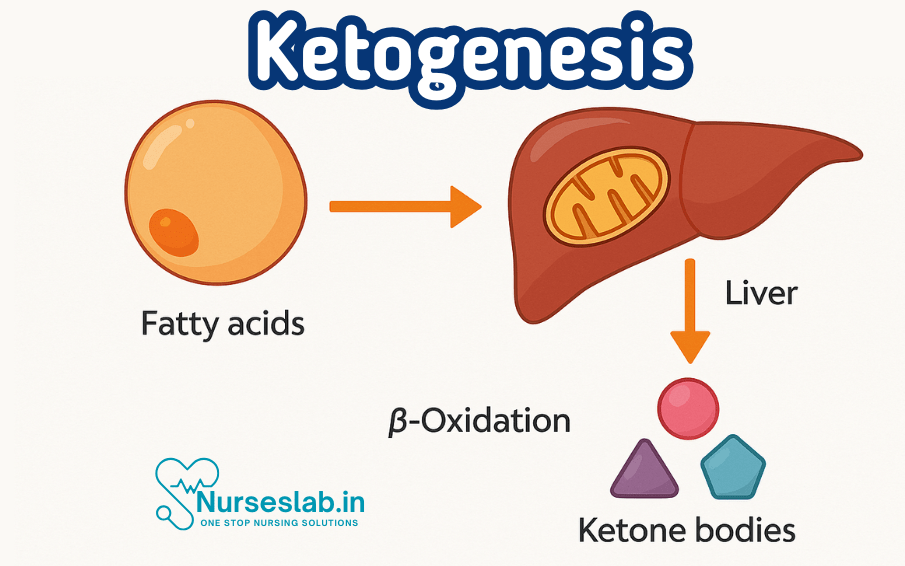
Ketogenesis is the metabolic process by which the liver converts fatty acids into ketone bodies. These ketone bodies—acetoacetate, beta-hydroxybutyrate, and acetone—serve as alternative energy sources when glucose is scarce, such as during fasting, prolonged exercise, or carbohydrate-restricted diets.
Historical Background
The concept of ketone body formation dates back to the 19th century, when scientists first observed their presence in the urine of patients with uncontrolled diabetes. Over time, research elucidated the pathways and regulatory mechanisms involved, highlighting ketogenesis as a vital adaptive response rather than merely a marker of disease.
Relevance to Nursing
For nurses, understanding ketogenesis is essential for managing patients with metabolic conditions, interpreting laboratory findings, and providing education on diet and lifestyle. It is particularly important in contexts such as diabetes management, critical care, paediatrics, and maternal health.
Biochemical Pathway of Ketogenesis
Key Enzymes and Substrates
Ketogenesis occurs primarily in the mitochondria of hepatocytes (liver cells). The process is initiated when the body’s stores of glycogen are depleted and fatty acids are mobilised from adipose tissue. The main substrates are free fatty acids, which are converted into acetyl-CoA via beta-oxidation.
The key enzymes involved in ketogenesis include:
- Acetyl-CoA acetyltransferase (thiolase): Catalyses the condensation of two acetyl-CoA molecules to form acetoacetyl-CoA.
- HMG-CoA synthase: Converts acetoacetyl-CoA and another acetyl-CoA to form HMG-CoA (3-hydroxy-3-methylglutaryl-CoA).
- HMG-CoA lyase: Cleaves HMG-CoA to yield acetoacetate, the first ketone body.
- Beta-hydroxybutyrate dehydrogenase: Interconverts acetoacetate and beta-hydroxybutyrate depending on the redox state.
Steps in the Liver
The process of ketogenesis unfolds as follows:
- Mobilisation of Fatty Acids: In response to low insulin and high glucagon levels, triglycerides in adipose tissue are broken down into free fatty acids.
- Beta-Oxidation: Fatty acids are transported to the liver and undergo beta-oxidation in the mitochondria, producing acetyl-CoA.
- Formation of Ketone Bodies: Excess acetyl-CoA is channelled into the ketogenesis pathway, forming acetoacetate, beta-hydroxybutyrate, and acetone.
- Release into Circulation: Ketone bodies are released into the bloodstream, where they are transported to peripheral tissues for energy utilisation.
Regulation of Ketogenesis
Ketogenesis is tightly regulated by hormonal and metabolic factors:
- Insulin: Inhibits lipolysis and ketogenesis. Low insulin levels, as seen in fasting or diabetes, promote ketone body formation.
- Glucagon: Stimulates ketogenesis by promoting fatty acid mobilisation and beta-oxidation.
- Substrate Availability: Increased fatty acid supply and acetyl-CoA concentrations favour ketone body synthesis.
This balance ensures that ketogenesis is activated only when necessary, preventing excessive accumulation of ketone bodies under normal circumstances.
Physiological Role of Ketone Bodies
Types of Ketone Bodies
There are three primary ketone bodies:
- Acetoacetate: The first ketone body formed during ketogenesis; it can be converted into the other ketone bodies or utilised directly for energy.
- Beta-hydroxybutyrate: Although technically not a true ketone, it is the most abundant in the blood and serves as a major energy substrate during prolonged fasting.
- Acetone: A volatile compound produced in smaller amounts, excreted mainly via the lungs and urine, responsible for the characteristic fruity odour in ketosis.
Energy Metabolism
Ketone bodies are vital alternative energy sources, especially for the brain, heart, and skeletal muscles during periods of glucose scarcity. Unlike fatty acids, ketone bodies can cross the blood-brain barrier, providing a critical fuel for the central nervous system when blood glucose levels are low.
Adaptation During Fasting and Starvation
During prolonged fasting or starvation, the body adapts by increasing ketone body production. This adaptation preserves muscle protein by reducing the need for gluconeogenesis from amino acids. The brain, which typically relies on glucose, progressively utilises ketone bodies, thereby conserving vital energy stores.
Clinical Significance
Ketosis
Ketosis refers to the physiological state in which there is an elevated concentration of ketone bodies in the blood. Mild ketosis can be observed during fasting, low-carbohydrate diets, or prolonged exercise and is generally considered a safe, adaptive response.
Ketoacidosis
Ketoacidosis is a pathological state characterised by a dangerous accumulation of ketone bodies, leading to metabolic acidosis. The most common form is diabetic ketoacidosis (DKA), seen in patients with type 1 diabetes mellitus due to absolute or relative insulin deficiency.
Key features of ketoacidosis include:
- Marked hyperglycaemia (in DKA)
- High anion gap metabolic acidosis
- Dehydration and electrolyte disturbances
- Presence of ketones in blood and urine
- Clinical symptoms: nausea, vomiting, abdominal pain, rapid breathing (Kussmaul respirations), fruity breath odour, confusion, and potential coma
Prompt recognition and management are essential, as untreated ketoacidosis can be life-threatening.
Ketogenesis in Diabetes
In patients with type 1 diabetes, insulin deficiency leads to unrestrained lipolysis and ketogenesis. Type 2 diabetes patients can also develop DKA under stress, infection, or other precipitating factors. Monitoring and managing ketone levels are thus crucial aspects of diabetes care.
Ketogenesis in Starvation
During starvation or very low-calorie diets, ketogenesis becomes the primary source of energy after glycogen stores are depleted. While physiological ketosis is generally safe, excessive or prolonged ketosis can have adverse effects, especially in vulnerable populations.
Pregnancy and Paediatric Considerations
Pregnant women are more susceptible to ketosis due to increased metabolic demands and altered hormonal profiles. Starvation or poorly controlled diabetes in pregnancy can lead to maternal and foetal complications. Similarly, children, especially infants, have limited glycogen reserves and can enter ketosis more rapidly during illnesses or fasting. Vigilance and early intervention are essential in these groups.
Nursing Assessment and Monitoring
Recognising Signs and Symptoms
Nurses play a pivotal role in identifying patients at risk of ketosis or ketoacidosis. Key signs and symptoms to monitor include:
- Polyuria, polydipsia, and weight loss
- Nausea, vomiting, abdominal pain
- Rapid, deep breathing (Kussmaul respirations)
- Altered mental status or confusion
- Fruity-smelling breath
Early recognition of these features can prompt timely investigations and interventions, reducing morbidity and mortality.
Laboratory Investigations
Essential laboratory tests for assessing ketogenesis and its complications include:
- Blood glucose levels
- Serum and urine ketone measurements
- Arterial or venous blood gas analysis for acidosis
- Electrolyte panel (sodium, potassium, bicarbonate)
- Anion gap calculation
Point-of-care ketone meters and dipsticks are valuable tools for rapid assessment, especially in emergency and community settings.
Patient Education
Nurses are often responsible for educating patients and families about the signs, risks, and management of ketosis and ketoacidosis. Education should encompass:
- Understanding the importance of blood glucose and ketone monitoring
- Recognising early warning signs
- When to seek medical attention
- Dietary advice, especially regarding carbohydrate intake and sick day rules in diabetes
Clear, empathetic communication can empower patients to take an active role in their care and prevent complications.
Management and Interventions
Nursing Care Plans
Nursing care for patients with ketosis or ketoacidosis should be individualised and comprehensive. Key components include:
- Frequent monitoring of vital signs, blood glucose, and ketones
- Assessment and maintenance of hydration status
- Electrolyte replacement as needed
- Administration of prescribed insulin (in DKA)
- Monitoring for complications such as cerebral oedema (especially in children)
- Psychosocial support and reassurance
Interdisciplinary collaboration with medical, dietary, and pharmacy teams enhances patient outcomes.
Dietary Considerations
Diet plays a crucial role in the management and prevention of abnormal ketogenesis. For patients at risk of ketosis, ensuring adequate carbohydrate intake is essential. In some settings, such as epilepsy management, ketogenic diets may be prescribed under specialist supervision. Nurses must be aware of the indications, benefits, and potential risks of such diets and support patients accordingly.
Emergency Management of Ketoacidosis
The management of diabetic ketoacidosis requires urgent intervention:
- Ensure airway, breathing, and circulation are stable.
- Initiate intravenous fluid resuscitation to correct dehydration.
- Administer insulin as per protocol to reduce blood glucose and suppress ketogenesis.
- Replace electrolytes, particularly potassium, which may drop rapidly with insulin therapy.
- Monitor for complications such as hypoglycaemia, cerebral oedema, and arrhythmias.
Nurses are central to the safe and effective delivery of these interventions, requiring vigilance, clinical judgement, and prompt communication with the multidisciplinary team.
Summary and Key Takeaways
Ketogenesis is a fundamental metabolic process with significant clinical implications for nursing practice. Understanding the biochemical pathway, physiological roles, and potential complications equips nurses to assess, monitor, and manage patients effectively. Key points include:
- Ketogenesis provides alternative energy during periods of glucose scarcity.
- Ketone bodies are essential for brain and muscle metabolism during fasting, starvation, or carbohydrate restriction.
- Pathological ketosis, especially ketoacidosis, is a medical emergency requiring prompt recognition and intervention.
- Nurses play a central role in assessment, monitoring, patient education, and management of ketogenesis-related conditions.
- Special considerations are necessary for vulnerable groups such as children and pregnant women.
A sound grasp of ketogenesis enhances nursing care, promotes patient safety, and supports positive health outcomes.
REFERENCES
- Harbans Lal, Textbook of Applied Biochemistry and Nutrition& Dietetics 2nd Edition ,November 2024, CBS Publishers and Distributors, ISBN: 978-9394525757
- Suresh K Sharma, Textbook of Biochemistry and Biophysics for Nurses, 2nd Edition, September 2022, Jaypee Publishers, ISBN: 978-9354655760
- Peter J Kennelly, Harpers Illustrated Biochemistry Standard Edition, September 2022, McGraw Hill Lange Publishers, ISBN: 978-1264795673
- Denise R Ferrier, Ritu Singh, Lippincott Illustrated Reviews Biochemistry, Second Edition, June 2024, ISBN- 978-8197055973
- Yadav, Tapeshwar & Bhadeshwar, Sushma. (2022). Essential Textbook of Biochemistry for Nursing.
- Applied Sciences, Importance of Biochemistry for Nursing Practice, November 2, 2023, https://bns.institute/applied-sciences/importance-biochemistry-nursing-practice/
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





