Introduction to Kidney Biopsy
A kidney biopsy is a vital medical procedure used in the diagnosis and management of various renal diseases. By extracting a small sample of kidney tissue for microscopic examination, clinicians can achieve a more precise understanding of the underlying cause of kidney dysfunction, tailor treatment strategies, and assess the progression or response to therapy.
What Is a Kidney Biopsy?
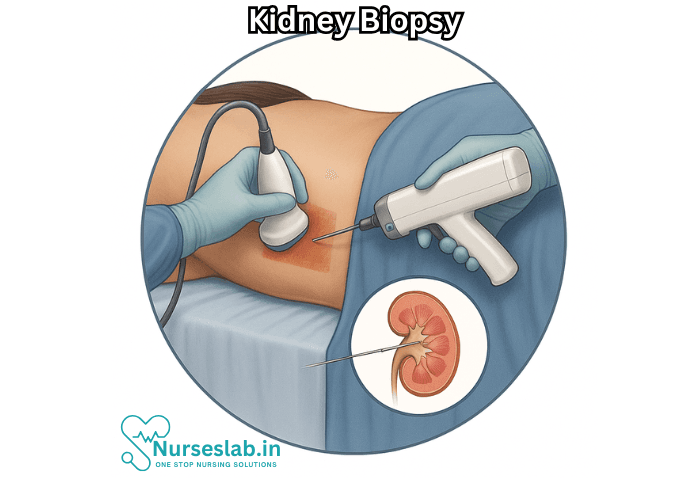
A kidney biopsy, medically termed renal biopsy, is the process of obtaining a tissue sample from the kidney. The sample is typically acquired by inserting a thin, hollow needle through the skin and into the kidney, a method known as percutaneous kidney biopsy. Less commonly, biopsies may be performed surgically, during procedures such as open or laparoscopic surgery. The tissue collected is then examined under a microscope, and may undergo additional laboratory tests, including immunofluorescence and electron microscopy.
Why Is a Kidney Biopsy Performed?
There are several critical reasons for conducting a kidney biopsy. These include:
- Diagnosing unexplained kidney problems: When routine blood, urine, and imaging tests cannot determine the cause of kidney dysfunction, a biopsy may provide definitive answers.
- Evaluating nephrotic syndrome: In cases where patients present with significant protein loss in urine, swelling, and abnormal kidney function, biopsy helps identify the specific disease affecting the kidney.
- Assessing hematuria or proteinuria: Persistent or unexplained blood or protein in the urine may necessitate a biopsy to identify underlying pathology.
- Monitoring transplanted kidneys: Biopsies can detect signs of rejection, infection, or other complications in kidney transplant recipients.
- Determining severity and progression of disease: Conditions such as glomerulonephritis, lupus nephritis, and other autoimmune kidney diseases are often assessed through biopsy to guide treatment.
- Guiding therapeutic decisions: The biopsy results allow physicians to personalize treatment, including immunosuppressive therapy or other targeted interventions.
Types of Kidney Biopsy Procedures
There are two main types of kidney biopsy procedures:
- Percutaneous (needle) biopsy: The most common method, performed under local anesthesia with ultrasound or CT guidance to ensure precise needle placement. It is minimally invasive and has a shorter recovery time.
- Open or laparoscopic surgical biopsy: Utilized when needle biopsy is not feasible or safe, often in patients with abnormal kidney anatomy, bleeding disorders, or those already undergoing surgery for another reason.
Preparation for Kidney Biopsy
Preparation is crucial for the safety and success of the kidney biopsy. Steps typically include:
- Pre-procedure evaluation: Patients undergo blood tests to assess clotting ability and kidney function. Imaging studies, such as ultrasound or CT scan, help map the kidneys.
- Medication review: Certain medications, especially blood thinners (e.g., warfarin, aspirin, clopidogrel), may need to be temporarily discontinued to reduce bleeding risk. Patients should notify their healthcare provider about all medications and supplements.
- Fasting: Some institutions require fasting prior to the procedure, particularly if sedation will be used.
- Consent: The procedure, risks, and benefits are explained, and written consent is obtained.
The Kidney Biopsy Procedure
The typical steps for a percutaneous kidney biopsy are as follows:
- Positioning: The patient lies on their abdomen (for native kidneys) or back (for transplanted kidneys).
- Sterilization and anesthesia: The skin over the kidney area is sterilized and numbed with local anesthetic.
- Imaging guidance: Ultrasound or CT imaging identifies the exact location of the kidney and guides needle placement.
- Needle insertion: A special biopsy needle is advanced into the kidney and a small piece of tissue is extracted, usually in one or more passes.
- Hemostasis: Immediate pressure is applied to the site to minimize bleeding.
- Sample handling: The tissue is preserved and sent to pathology for analysis.
After the Procedure: Recovery and Monitoring
Following a kidney biopsy, patients are closely monitored for several hours to detect and manage any complications. Typical post-biopsy care includes:
- Bed rest: Patients may need to remain in bed for 4-6 hours after the procedure to reduce the risk of bleeding.
- Vital signs monitoring: Regular checks of blood pressure, pulse, and urine output are performed.
- Urine monitoring: Observation for blood in the urine, which can occur temporarily after the procedure.
- Pain management: Mild discomfort or soreness at the biopsy site is common and usually managed with over-the-counter pain relievers.
- Follow-up: Patients are typically advised to avoid strenuous activity and heavy lifting for several days.
Potential Risks and Complications
While kidney biopsy is generally safe, it is not without risks. The most common complications include:
- Bleeding: The most frequent complication, ranging from minor (blood in urine) to rarely severe (requiring transfusion or intervention).
- Pain or discomfort: Usually mild and transient.
- Infection: Risk is low, but any signs of fever or worsening pain should be reported.
- Injury to surrounding organs: Rarely, the needle may damage other organs or structures.
- Arteriovenous fistula: An abnormal connection between an artery and vein within the kidney, which typically resolves spontaneously.
Interpreting the Results
Once the kidney tissue sample is analyzed in the pathology laboratory, a detailed report is generated. The report may include:
- Diagnosis: Identification of the specific kidney disease (e.g., glomerulonephritis, minimal change disease, diabetic nephropathy, lupus nephritis).
- Severity and extent: Assessment of how advanced or severe the disease is, and involvement of different kidney structures.
- Prognosis: Estimation of likely disease progression and response to therapy.
- Treatment guidance: Recommendations for medications, lifestyle changes, or further interventions.
Who Needs a Kidney Biopsy?
Kidney biopsy is not performed in every case of kidney disease. It is generally reserved for situations where the diagnosis is unclear or when precise pathology is needed to guide management. Common indications include:
- Unexplained acute or chronic kidney failure
- Significant proteinuria or nephrotic syndrome
- Persistent hematuria
- Suspected autoimmune or inflammatory renal disease
- Monitoring complications in kidney transplant recipients
Some patients may not be suitable candidates for biopsy due to bleeding disorders, uncontrolled hypertension, solitary kidney, or active infection.
Alternatives to Kidney Biopsy
While biopsy remains the gold standard for kidney diagnosis, alternative, less invasive tests may be used in certain circumstances:
- Blood and urine tests for markers of renal injury
- Imaging studies, such as ultrasound, CT, or MRI
- Genetic and serological tests in hereditary or autoimmune conditions
However, these alternatives may not provide the detailed information obtained by direct tissue analysis.
Nursing Care of Patients Undergoing Kidney Biopsy
A kidney biopsy, also known as a renal biopsy, is a diagnostic procedure that involves obtaining a small sample of kidney tissue for microscopic examination. This procedure plays a crucial role in diagnosing, evaluating, and managing a wide spectrum of renal diseases, including nephrotic syndrome, glomerulonephritis, unexplained renal failure, and transplant rejection. As with any invasive procedure, it carries certain risks, most notably bleeding, infection, and injury to the kidney. Nursing care before, during, and after the biopsy is vital for ensuring patient safety and optimal outcomes.
Pre-Procedure Nursing Care
1. Patient Education
- Explain the purpose and process of the kidney biopsy to the patient, including its benefits and potential risks, to alleviate anxiety and encourage cooperation.
- Discuss the expected sensations during the procedure (e.g., local anesthetic sting, pressure during tissue retrieval).
- Review any specific instructions, such as fasting requirements or discontinuation of certain medications (especially anticoagulants, aspirin, NSAIDs) as directed by the physician.
2. Informed Consent
- Ensure that informed consent is obtained and properly documented in the patient’s medical record.
- Clarify any doubts the patient or family may have about the procedure.
3. Pre-Procedure Assessments and Preparation
- Obtain a detailed medical, surgical, and medication history, focusing on coagulopathies, bleeding disorders, hypertension, and allergies.
- Review laboratory results: specifically, check complete blood count (CBC), coagulation profile (PT, INR, aPTT), serum creatinine, and blood urea nitrogen (BUN) to ensure the patient is a suitable candidate for biopsy.
- Check vital signs and baseline observations.
- Ensure an intravenous line is established for emergency access if needed.
- Ask the patient to void prior to the procedure to reduce the bladder’s risk of being punctured.
- Remove jewelry or metallic objects from the area to be biopsied to reduce imaging artifacts.
Intra-Procedure Nursing Care
1. Positioning and Monitoring
- Assist the patient into the required position, usually prone (face down) with a pillow under the abdomen, or supine for transplanted kidneys.
- Monitor the patient’s vital signs continuously throughout the procedure.
- Provide emotional support, reassurance, and clear communication to the patient to minimize anxiety.
2. Maintaining Aseptic Technique
- Ensure strict adherence to aseptic technique to minimize the risk of infection during needle insertion and tissue collection.
3. Support During Biopsy
- Instruct the patient to remain still and hold their breath momentarily as directed by the physician when the biopsy needle is inserted. This helps prevent accidental injury to the kidney or surrounding structures.
- Be prepared to assist the physician with specimen collection and handling.
- Observe for signs of immediate complications, such as severe pain, hypotension, tachycardia, or visible bleeding at the puncture site.
Post-Procedure Nursing Care
1. Immediate Post-Biopsy Care
- Monitor vital signs (blood pressure, pulse, respiratory rate, temperature) every 15 minutes for the first hour, every 30 minutes for the next two hours, and then hourly for at least the next four hours or as per institutional protocol.
- Assess for signs of bleeding (flank pain, hypotension, tachycardia, a drop in hemoglobin and hematocrit, gross hematuria) and infection (fever, chills, redness or swelling at puncture site).
- Inspect the puncture site regularly for external bleeding or hematoma formation.
- Encourage the patient to remain on strict bed rest in the supine position for at least 4–6 hours post-procedure, or longer if indicated due to complications or per local policy.
- Maintain a pressure dressing over the biopsy site to minimize risk of bleeding.
2. Pain and Comfort Management
- Administer prescribed analgesics as needed to relieve mild to moderate pain or discomfort.
- Monitor for and report severe or persistent pain promptly, as it may indicate internal bleeding or other complications.
3. Fluid and Dietary Management
- Monitor and record intake and output meticulously. Ensure adequate hydration unless contraindicated.
- Observe for hematuria (bloody urine), especially within the first 24 hours.
- Restrict heavy meals until the patient is fully alert post-procedure. Offer light, easily digestible foods initially.
4. Patient Education and Discharge Planning
- Educate the patient on the importance of continued rest and activity restrictions following discharge (typically 24–48 hours).
- Advise to avoid strenuous physical activities, lifting heavy objects, or vigorous exercise for at least 1 to 2 weeks to prevent bleeding.
- Instruct the patient to monitor for and immediately report warning signs such as persistent hematuria, severe flank or abdominal pain, dizziness, weakness, fever, chills, or signs of infection at the puncture site.
- Provide clear written and verbal instructions regarding follow-up appointments, wound care, activity, and medication use.
Potential Complications and Emergency Management
- Bleeding: The most common complication. Monitor for signs of internal or external bleeding and intervene promptly (administer IV fluids, blood transfusion, or surgical intervention as ordered).
- Infection: Maintain aseptic technique and monitor puncture site. Treat early signs of infection with antibiotics as prescribed.
- Hematuria: Transient microscopic hematuria is common; persistent or gross hematuria requires immediate reporting to the physician.
- Arteriovenous fistula formation: Rare, but may present with bruit or thrill over biopsy site; requires specialist referral.
- Other rare complications: Include injury to adjacent organs, hypertension, and allergic reactions to medications or antiseptics.
Documentation
- Record all observations, including baseline and subsequent vital signs, assessment findings, patient responses, and interventions carried out.
- Document the patient’s understanding of post-procedure care and discharge instructions.
- Note the number of tissue samples taken, the condition of the biopsy site, and any complications or unusual findings.
REFERENCES
- Dirkx TC, Woodell TB. Kidney Biopsy. In: Papadakis MA, McPhee SJ, Rabow MW, et al., eds. Current Medical Diagnosis & Treatment 2024. McGraw Hill; 2024.
- Feehally J, et al., eds. Renal biopsy. In: Comprehensive Clinical Nephrology. 6th ed. Elsevier; 2019. https://www.clinicalkey.com
- Yu ASL, et al., eds. The renal biopsy. In: Brenner & Rector’s The Kidney. 11th ed. Elsevier; 2020. https://www.clinicalkey.com.
- Hogan JJ, Mocanu M, Berns JS. The Native Kidney Biopsy: Update and Evidence for Best Practice. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4741037/). Clin J Am Soc Nephrol. 2016 Feb 5;11(2):354-62.
- Hull KL, Adenwalla SF, Topham P, Graham-Brown MP. Indications and considerations for kidney biopsy: an overview of clinical considerations for the non-specialist. Clin Med (Lond). 2022 Jan;22(1):34-40. doi: 10.7861/clinmed.2021-0472. Epub 2021 Dec 17.
- Luciano RL, Moeckel GW. Update on the Native Kidney Biopsy: Core Curriculum 2019 (https://pubmed.ncbi.nlm.nih.gov/30661724/). Am J Kidney Dis. 2019;73(3):404-415.
- Merck Manual. Biopsy of the Kidneys, Bladder, and Prostate https://www.merckmanuals.com/professional/genitourinary-disorders/genitourinary-tests-and-procedures/biopsy-of-the-kidneys,-bladder,-and-prostate. Updated 9/2022.
- National Institute of Diabetes and Digestive and Kidney Diseases (U.S.). Kidney Biopsy. https://www.niddk.nih.gov/health-information/diagnostic-tests/kidney-biopsy. Updated 3/2022.
- National Kidney Foundation. Kidney Biopsy. https://www.kidney.org/atoz/content/kidney-biopsy.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





