A salivary gland scan is a nuclear medicine test that evaluates the function and drainage of the salivary glands. It helps detect obstruction, inflammation, infection, and tumors. Understanding indications, procedure steps, and interpretation is essential in ENT and diagnostic imaging.
Introduction
The salivary glands play a vital role in the digestive system, producing saliva that aids in digestion, protects oral tissues, and maintains oral hygiene. When these glands are affected by disease or dysfunction, it can lead to symptoms such as swelling, pain, dry mouth, or infections. Diagnosing salivary gland disorders accurately is crucial for effective management, and one of the key diagnostic tools used is the salivary gland scan.
Purpose and Indications
What is a Salivary Gland Scan?
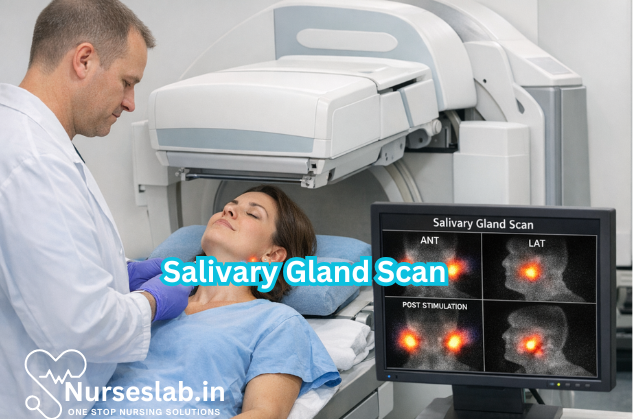
A salivary gland scan, also known as salivary scintigraphy, is a non-invasive nuclear medicine imaging technique used to assess the function and structure of the salivary glands. The scan involves the administration of a small amount of radioactive tracer, typically technetium-99m pertechnetate, which is taken up by the salivary glands and excreted into the mouth. Special cameras (gamma cameras) capture images that help physicians evaluate gland function, detect obstructions, inflammation, or tumours, and monitor treatment response.
Why and When is the Scan Used?
- Diagnosis of Salivary Gland Dysfunction: To assess reduced or abnormal function in conditions such as Sjögren’s syndrome, chronic sialadenitis, or radiation-induced damage.
- Detection of Obstructions: To identify blockages in the salivary ducts caused by stones (sialolithiasis) or strictures.
- Evaluation of Masses or Tumours: To characterise the nature of glandular swellings and differentiate between benign and malignant processes.
- Assessment of Inflammatory Conditions: To distinguish between acute and chronic inflammation and monitor response to therapy.
- Pre- and Post-Treatment Evaluation: To establish baseline gland function before interventions and track recovery or progression after treatment.
Preparation for the Salivary Gland Scan
Proper preparation is essential to ensure optimal scan results and patient safety. The following outlines the typical steps involved in preparing for a salivary gland scan:
Patient Instructions
- Fasting: Patients are usually advised to avoid eating, drinking, or chewing gum for two to four hours before the scan. This prevents external stimulation of the glands and ensures accurate baseline measurements.
- Medication Review: Certain medications, such as anticholinergics or antihistamines, may affect salivary gland function. Patients should inform their doctor about all medications being taken. Some drugs may need to be paused temporarily under medical supervision.
- Hydration: Patients may be instructed to drink water before the scan to avoid dehydration, unless otherwise directed.
- Oral Hygiene: Good oral hygiene is encouraged to reduce the risk of infection, but patients should avoid using mouthwashes that contain alcohol or strong antiseptics on the day of the scan.
- Pregnancy and Breastfeeding: Women who are pregnant, planning pregnancy, or breastfeeding should inform the healthcare team, as radioactive tracers may not be recommended in these situations.
- Clothing and Accessories: Comfortable clothing is advised, and patients may be asked to remove jewellery or dental appliances that could interfere with imaging.
Consent and Explanation
Before the procedure begins, the healthcare provider will explain the scan process, answer any questions, and obtain informed consent.
Step-by-Step Procedure
1. Arrival and Registration
Upon arrival, patients check in at the imaging centre. Identification details are verified, and the procedure is reviewed once again.
2. Intravenous Administration of Radiotracer
A small amount of radioactive tracer (commonly technetium-99m pertechnetate) is injected into a vein, usually in the arm. The dose is low and specifically calculated for diagnostic purposes.
3. Initial Imaging (Uptake Phase)
After injection, the patient is positioned comfortably on an imaging table, with the head and neck area aligned under a gamma camera. The camera detects the radiation emitted by the tracer as it is taken up by the salivary glands (parotid, submandibular, and sublingual).
Serial images are taken every 20–30 seconds for the first 15–20 minutes. This phase assesses the ability of the glands to concentrate the tracer from the bloodstream.
4. Stimulation and Excretion Phase
After the uptake phase, the patient is asked to suck on a sour substance, such as lemon juice or a citric acid tablet. This stimulates the salivary glands to secrete saliva, which in turn causes the tracer to be excreted into the mouth.
Further images are obtained over the next 10–15 minutes to evaluate the excretory function of the glands. This dynamic imaging allows for assessment of both uptake and drainage efficiency.
5. Monitoring and Completion
Throughout the procedure, the patient is monitored for comfort and any adverse reactions. The entire scan typically takes 30–45 minutes. Once imaging is complete, the intravenous line is removed, and the patient is allowed to leave unless further observation is required.
Interpretation of Results
A nuclear medicine specialist or radiologist interprets the images by analysing the pattern of tracer uptake and excretion in each gland. The following outlines the typical findings:
- Normal Scan: All major salivary glands show prompt, symmetrical uptake of tracer, followed by rapid excretion after stimulation.
- Obstructive Pattern: A gland may show normal uptake but delayed or reduced excretion, indicating a blockage (e.g., stone or duct stricture).
- Inflammatory Pattern: Diffuse reduction in tracer uptake and excretion, often seen in chronic sialadenitis or autoimmune conditions like Sjögren’s syndrome.
- Mass Lesions: Focal areas of absent or reduced uptake may suggest a tumour or cyst, warranting further anatomical imaging.
- Post-Treatment Changes: Reduced function or altered uptake patterns may be observed after surgery, radiation, or other therapies.
Risks and Benefits
Benefits
- Functional Assessment: The scan provides unique information about gland activity that cannot be obtained from anatomical imaging alone.
- Non-Invasive: The procedure does not require surgery or tissue sampling.
- Minimal Discomfort: Only a small injection is required, and the scan is generally well tolerated.
- Guidance for Treatment: Helps clinicians plan interventions and monitor response to therapy.
- Low Radiation Exposure: The tracer used emits low levels of radiation, minimising risk to the patient.
Risks
- Radiation Exposure: Although the radiation dose is low, unnecessary scans should be avoided, especially in children and pregnant women.
- Allergic Reactions: Rarely, patients may experience mild allergic reactions to the tracer, such as rash or itching.
- Discomfort or Bruising: At the injection site, minor pain or bruising may occur.
- False Positives/Negatives: As with any diagnostic test, there is a chance of inaccurate results due to technical factors or overlapping conditions.
Overall, the benefits of accurate diagnosis and functional assessment generally outweigh the minimal risks associated with the procedure.
Post-Procedure Care
After completion of the salivary gland scan, patients can usually resume normal activities immediately.
- Hydration: Drink plenty of fluids for the next 24 hours to help flush the radioactive tracer from the body.
- Breastfeeding: If breastfeeding, consult the nuclear medicine team. It may be advised to discard breast milk for a short period after the scan to prevent infant exposure to the tracer.
- Monitor for Side Effects: While side effects are rare, patients should report any unusual symptoms (such as rash, swelling, or difficulty breathing) to their healthcare provider.
- Radiation Precautions: The level of radiation is low and does not pose a risk to household contacts, but patients should follow any specific instructions given by the medical team.
- Follow-Up: Results are typically reviewed at a follow-up appointment. Further tests or treatments may be planned based on the findings.
Nursing Care of Patients Undergoing Salivary Gland Scan Procedure
As nurses play an integral role in ensuring patient safety and comfort throughout the procedure, it is essential to understand the specific aspects of care before, during, and after a salivary gland scan.
Pre-Procedure Nursing Care
Patient Assessment
Prior to the scan, the nurse should conduct a thorough assessment, including:
- Reviewing the patient’s medical history for allergies, pregnancy, or prior reactions to contrast agents
- Assessing renal function, as impaired excretion may affect tracer clearance
- Checking for any medications that may interfere with salivary gland function (e.g., anticholinergics)
- Evaluating the patient’s ability to understand and comply with instructions
Patient Preparation
Effective patient preparation minimizes anxiety and ensures optimal scan results:
- Informed Consent: Explain the procedure, risks, and benefits. Obtain written consent as per hospital policy.
- Fasting: Some protocols require fasting for 2–4 hours before the scan to optimize tracer uptake and gland visualization. Confirm with the radiology department.
- Medication Review: Advise the patient to avoid medications that may affect salivary gland function, as directed by the physician.
- Hydration: Encourage adequate hydration unless contraindicated.
- Oral Hygiene: Instruct the patient to maintain good oral hygiene prior to the scan to reduce infection risk and ensure clear imaging.
- Explanation: Reassure the patient that the procedure is minimally invasive and that the radioactive tracer is safe with negligible side effects.
- Pregnancy Testing: For women of childbearing age, ensure pregnancy status is confirmed before proceeding.
Environmental Preparation
- Prepare a quiet, comfortable, and well-lit environment in the imaging department.
- Ensure necessary equipment is available: intravenous supplies, radiopharmaceuticals, gamma camera, and emergency equipment.
- Check for any contraindications or special precautions as per the physician’s orders.
Intra-Procedure Nursing Care
Patient Positioning and Comfort
- Assist the patient to lie supine on the scanning table with the head slightly extended for optimal gland visualization.
- Provide pillows or supports to enhance comfort and minimize movement during the scan.
- Encourage relaxation and stillness throughout the procedure to prevent image artifacts.
Administration of Radiopharmaceutical
- Ensure correct identification of the patient and the radiopharmaceutical agent.
- Administer the tracer intravenously, adhering strictly to safety protocols for handling radioactive materials.
- Monitor for immediate adverse reactions, such as allergic responses or extravasation at the injection site.
- Document time and dose of tracer administration.
Monitoring During Imaging
- Observe the patient for signs of discomfort, anxiety, or adverse reactions.
- Maintain verbal communication with the patient, providing reassurance as needed.
- Assist in administering sialogogues (e.g., lemon juice or citric acid) if required to stimulate gland secretion during the scan.
- Record any events or interventions during the procedure.
Post-Procedure Nursing Care
Immediate Post-Scan Care
- Assess the patient for delayed reactions to the radiopharmaceutical.
- Remove intravenous lines and apply pressure to the site, ensuring hemostasis.
- Encourage oral intake of fluids to facilitate tracer excretion and reduce radiation exposure.
- Provide oral hygiene instructions to maintain cleanliness and comfort.
- Monitor for signs of infection or inflammation at the injection site.
Patient Education and Discharge Instructions
- Advise the patient that the radioactive tracer will be eliminated primarily through urine, and that increased fluid intake will help speed up this process.
- Inform the patient to report any unusual symptoms, such as rash, swelling, or difficulty swallowing.
- Explain that results will be reviewed by the radiologist and communicated by the referring physician.
- Provide instructions on when normal activities can be resumed; typically, there are no restrictions post-scan.
- Emphasize the importance of follow-up appointments for further evaluation or treatment based on scan findings.
Documentation
- Record all relevant details in the patient’s medical chart, including assessment, consent, medication administration, procedure events, and post-procedure status.
- Document any adverse reactions, interventions, and discharge teaching provided.
Special Considerations
Pediatric Patients
- Use age-appropriate explanations and comfort measures.
- Involve parents or caregivers in preparation and support.
- Utilize distraction techniques or mild sedation if necessary.
Geriatric Patients
- Assess for comorbidities and polypharmacy that may impact procedure safety.
- Provide additional support for mobility and positioning.
- Monitor closely for dehydration or delayed tracer excretion.
Patients with Special Needs
- Adapt communication and comfort strategies for patients with sensory, cognitive, or physical impairments.
- Coordinate with multidisciplinary teams for optimal care.
Infection Control and Radiation Safety
Nurses must adhere to strict infection control and radiation safety protocols:
- Use gloves and aseptic technique during intravenous administration.
- Dispose of radioactive materials according to institutional and regulatory guidelines.
- Limit exposure to radiation for staff and other patients by following time, distance, and shielding principles.
- Educate patients about radiation safety and dispel common myths or fears.
Complications and Emergency Management
- Allergic Reactions: Be prepared to manage rare allergic responses to radiopharmaceuticals, with access to emergency medications and equipment.
- Extravasation: If tracer leaks into surrounding tissue, stop the injection, apply local care, and notify the physician.
- Anxiety or Claustrophobia: Provide emotional support, offer sedation if prescribed, and communicate clearly throughout the procedure.
REFERENCES
- Chen YC, Chen HY, Hsu CH. Recent Advances in Salivary Scintigraphic Evaluation of Salivary Gland Function. Diagnostics (Basel). 2021 Jun 28;11(7):1173. doi: 10.3390/diagnostics11071173. PMID: 34203365; PMCID: PMC8305115.
- Loutfi I, Nair MK, Ebrahim AK. Salivary gland scintigraphy: the use of semiquantitative analysis for uptake and clearance (https://pubmed.ncbi.nlm.nih.gov/12777459/). J Nucl Med Technol. 2003;31(2):81-5.
- Benito, D.A., Badger, C., Hoffman, H.T. et al. Recommended Imaging for Salivary Gland Disorders. Curr Otorhinolaryngol Rep 8, 311–320 (2020). https://doi.org/10.1007/s40136-020-00299-2
- An, Y.-S., Lee, S. J., Jung, J.-Y., & Yoon, J.-K. (2022). Sublingual Gland Observed on Salivary Gland Scan. Clinical Nuclear Medicine, 47(10), 876–877. https://doi.org/10.1097/RLU.0000000000004183
- MyHealthAlberta.ca. Salivary Gland Scan https://myhealth.alberta.ca/Health/Pages/conditions.aspx?hwid=hw234444. Current as of 12/18/2022.
- Wang KY, Wintermark M, Penta M. Imaging characteristics of Sjögren’s syndrome (https://pubmed.ncbi.nlm.nih.gov/36137442/). Clin Imaging. 2022 Dec;92:7-18. Accessed 6/12/2024.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





