Introduction
Atrial arrhythmias are a group of abnormal heart rhythms that originate from the atria, the upper chambers of the heart. These disturbances in the electrical activity of the atria can significantly affect the heart’s ability to effectively pump blood, potentially leading to a range of symptoms and complications. Atrial arrhythmias are common, particularly in older adults, and include various forms such as atrial fibrillation, atrial flutter, and atrial tachycardia. Due to their prevalence and possible association with serious outcomes like stroke and heart failure, understanding atrial arrhythmias is crucial for both patients and healthcare providers.
The Normal Cardiac Conduction System
To appreciate the impact of atrial arrhythmias, it is essential to understand the normal electrical conduction in the heart. The heart’s rhythm is dictated by electrical impulses originating from the sinoatrial (SA) node, also known as the heart’s natural pacemaker, located in the right atrium. These impulses travel through the atria, causing them to contract and push blood into the ventricles. The impulse then passes through the atrioventricular (AV) node and into the ventricles, ensuring coordinated heartbeats. Any disturbance in this process, particularly in the atria, can result in arrhythmias.
Types of Atrial Arrhythmias
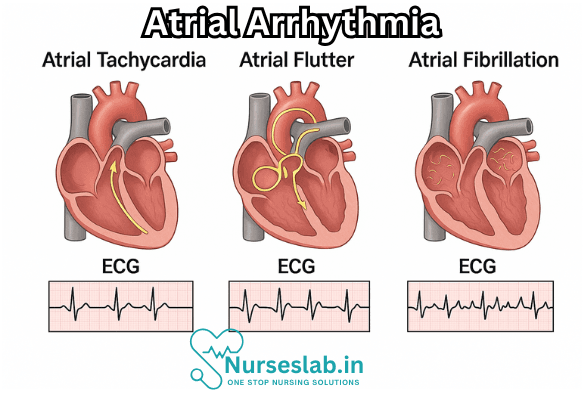
- Atrial Fibrillation (AF): This is the most common type of atrial arrhythmia. It is characterized by rapid, chaotic electrical impulses in the atria, leading to irregular and often fast heartbeats. The atria quiver instead of contracting effectively, increasing the risk of blood clots, stroke, and heart failure.
- Atrial Flutter: Similar to atrial fibrillation but more organized, atrial flutter features a rapid, regular rhythm. The electrical signals travel in a circular pathway within the right atrium, causing the atria to beat rapidly but regularly.
- Atrial Tachycardia: This refers to a rapid heartbeat originating from a focus within the atria other than the SA node. It can be due to a single site (focal atrial tachycardia) or multiple sites (multifocal atrial tachycardia).
- Supraventricular Tachycardia (SVT): Although not exclusively atrial, certain types of SVT originate in the atria or involve atrial tissue, leading to episodes of rapid heart rate.
Causes and Risk Factors
Atrial arrhythmias result from abnormalities in the electrical properties or structure of the atria. Common causes and risk factors include:
- Advancing Age: The risk of atrial arrhythmias increases with age due to changes in cardiac tissue.
- Hypertension (High Blood Pressure): Long-standing high blood pressure can enlarge and scar the atria, increasing arrhythmia risk.
- Coronary Artery Disease: Blockages in the heart’s arteries can compromise blood supply to the atria.
- Heart Failure: Weakened heart muscle disrupts electrical conduction.
- Valvular Heart Disease: Especially mitral valve disorders, which can strain the left atrium.
- Thyroid Disorders: Overactive thyroid (hyperthyroidism) can precipitate arrhythmias.
- Alcohol Use: Excessive or binge drinking can trigger atrial arrhythmias (“holiday heart syndrome”).
- Sleep Apnea: Recurrent drops in oxygen during sleep stress the heart and increase arrhythmia risk.
- Obesity and Diabetes: Both are linked to greater risk of atrial arrhythmias.
- Genetic Predisposition: Family history may increase susceptibility.
- Other Factors: Infections, lung diseases, stimulant drugs, and some medications may contribute.
Signs and Symptoms
The clinical presentation of atrial arrhythmias varies widely. Some individuals may remain asymptomatic, while others experience pronounced symptoms, including:
- Palpitations (sensation of a racing, fluttering, or irregular heartbeat)
- Fatigue or weakness
- Dizziness or lightheadedness
- Shortness of breath
- Chest pain or discomfort
- Fainting (syncope), particularly in severe cases
- Reduced exercise tolerance
It is important to note that some people with atrial arrhythmias (especially atrial fibrillation) may be unaware of their condition until a complication, such as a stroke, occurs.
Potential Complications
Atrial arrhythmias can have significant consequences if left untreated:
- Stroke: Ineffective atrial contractions can cause blood stasis and clot formation, particularly in atrial fibrillation. If a clot travels to the brain, it can cause a stroke.
- Heart Failure: Prolonged rapid or irregular heart rhythms may weaken the heart muscle.
- Thromboembolism: Blood clots that form in the atria may travel to other parts of the body, causing organ damage.
- Reduced Quality of Life: Symptoms can interfere with daily activities and overall wellbeing.
Diagnosis of Atrial Arrhythmias
Diagnosis begins with a thorough clinical evaluation, including:
- Medical History and Physical Examination: Assessing symptoms, risk factors, and any underlying heart disease.
- Electrocardiogram (ECG): The primary tool for identifying the type of arrhythmia by recording the heart’s electrical activity.
- Holter Monitoring: A portable device that records continuous ECG data over 24-48 hours to detect intermittent arrhythmias.
- Event Recorder or Loop Recorder: Used for longer-term monitoring when symptoms are infrequent.
- Echocardiogram: An ultrasound of the heart to assess its structure and function.
- Blood Tests: Can identify contributing factors such as thyroid dysfunction or electrolyte imbalances.
- Other Tests: Stress testing, cardiac MRI, or CT scan may be needed in some cases.
Management and Treatment
The treatment of atrial arrhythmias is tailored to the specific type, severity, symptoms, and underlying causes. The primary goals are to restore and maintain a normal heart rhythm, control heart rate, prevent complications, and improve quality of life. Main approaches include:
Lifestyle Modifications
- Limiting alcohol and caffeine intake
- Managing stress and improving sleep hygiene
- Controlling blood pressure and blood sugar
- Maintaining a healthy weight
- Treating sleep apnea if present
- Engaging in regular physical activity as recommended
Medications
- Rate Control Medications: Beta-blockers, calcium channel blockers, and digoxin can slow the heart rate.
- Rhythm Control Medications (Antiarrhythmics): Drugs such as flecainide, amiodarone, or sotalol may help restore and maintain normal rhythm.
- Anticoagulants (Blood Thinners): To reduce the risk of blood clots and stroke, especially in atrial fibrillation. Options include warfarin, dabigatran, rivaroxaban, and apixaban.
Non-Pharmacological Interventions
- Electrical Cardioversion: A procedure that uses controlled electric shocks to restore normal rhythm, often used for atrial fibrillation or flutter.
- Catheter Ablation: A minimally invasive technique where abnormal electrical pathways in the heart are destroyed using radiofrequency energy or cryotherapy.
- Pacemaker Implantation: For some arrhythmias, especially if the heart rate becomes too slow, a pacemaker may be required.
- Surgical Approaches: In some cases, surgery such as the Maze procedure is performed to create scar tissue that interrupts abnormal signals.
Prevention of Stroke
The prevention of thromboembolic complications is especially important for patients with atrial fibrillation. Risk assessment tools like the CHA₂DS₂-VASc score help determine the need for anticoagulation therapy.
Living with Atrial Arrhythmia
A diagnosis of atrial arrhythmia can be concerning, but with appropriate care, many individuals lead full and active lives. Regular follow-up, adherence to treatment, and awareness of symptoms are essential. Advances in medical therapies and procedures continue to improve outcomes.
Nursing Care of Patients with Atrial Arrhythmia
Therapeutic Interventions
- Medication Administration: Administer prescribed antiarrhythmic drugs, anticoagulants (such as warfarin or DOACs), beta-blockers, calcium channel blockers, or digoxin. Monitor for side effects and ensure timely dosing.
- Oxygen Therapy: Provide supplemental oxygen if hypoxia is present or patient is breathless.
- Electrical Cardioversion: Prepare and assist in procedures like electrical cardioversion if indicated and ordered by the physician. Ensure informed consent is obtained and patient is adequately sedated.
- Fluid Management: Monitor and regulate intravenous fluids to prevent overload, especially in patients at risk of heart failure.
Patient Education
- Medication Compliance: Educate patients about the importance of taking medications as prescribed, possible side effects, and regular follow-up.
- Lifestyle Modifications: Advise on reducing caffeine, avoiding alcohol, quitting smoking, and maintaining a heart-healthy diet low in salt and fat.
- Recognising Warning Signs: Teach patients and family members to recognise symptoms such as palpitations, chest pain, breathlessness, or fainting, and when to seek immediate medical help.
- Activity Guidance: Encourage moderate activity as tolerated, but advise avoidance of strenuous exercise until cleared by the physician.
Prevention of Complications
- Stroke Prevention: Ensure anticoagulation therapy is maintained to reduce the risk of thromboembolism and stroke, especially in atrial fibrillation.
- Infection Control: Maintain aseptic techniques during invasive procedures and monitor for signs of infection, especially in those with implanted devices.
- Pressure Ulcer Prevention: For bed-ridden patients, implement regular position changes and skin care.
Psychosocial Support
- Emotional Support: Be empathetic and supportive, as arrhythmia can cause significant anxiety and fear. Provide reassurance and answer questions patiently.
- Counselling: Refer to counselling services if needed for coping with chronic illness and lifestyle changes.
- Family Involvement: Involve family in education and care planning to ensure adequate support at home.
Documentation
- Accurate Records: Document all assessments, interventions, patient responses, and education provided.
- Incident Reporting: Report any adverse events, medication errors, or new symptoms promptly according to hospital policy.
REFERENCES
- American Heart Association (AHA). About Arrhythmia. https://www.heart.org/en/health-topics/arrhythmia/about-arrhythmia
- Jalife J, et al., eds. Assessment of the patient with a cardiac arrhythmia. In: Zipes and Jalife’s Cardiac Electrophysiology: From Cell to Bedside. 8th ed. Elsevier; 2022. https://www.clinicalkey.com.
- American Heart Association (AHA). Atrial Fibrillation. https://www.heart.org/en/health-topics/atrial-fibrillation.
- Merck Manual (Consumer Version). Atrial Premature Beats. https://www.merckmanuals.com/home/heart-and-blood-vessel-disorders/abnormal-heart-rhythms/atrial-premature-beats
- Libby P, et al., eds. Approach to the patient with cardiac arrhythmias. In: Braunwald’s Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Elsevier; 2022. https://www.clinicalkey.com.
- National Heart, Lung, and Blood Institute. Arrhythmia. https://www.nhlbi.nih.gov/health-topics/arrhythmia.
- Cronin EM, et al. 2019 HRS/EHRA/APHRS/LAHRS expert consensus statement on catheter ablation of ventricular arrhythmias. Heart Rhythm. 2020; doi:10.1016/j.hrthm.2019.03.002.
- Tisdale JE, et al. Drug-induced arrhythmias: A scientific statement from the American Heart Association. Circulation. 2020; doi:10.1161/CIR.0000000000000905.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





