Introduction
Elbow replacement surgery, also known as total elbow arthroplasty, is a medical procedure designed to replace the damaged or diseased parts of the elbow joint with artificial components. This surgery is typically recommended for individuals suffering from severe arthritis, significant fractures, or other conditions that severely impair elbow function and cause chronic pain.
Understanding Elbow Anatomy
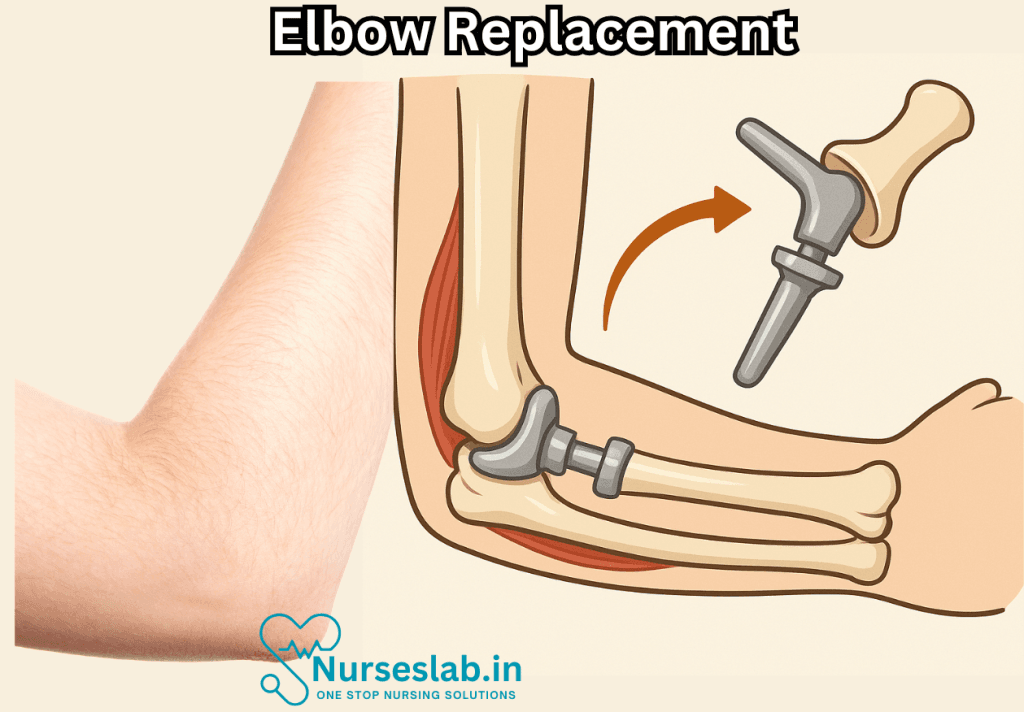
The elbow is a complex hinge joint that connects the upper arm bone (humerus) to the two bones of the forearm (radius and ulna). The joint’s unique structure allows for a combination of hinge and pivot movements, providing the arm with flexibility and strength. The smooth cartilage that covers the ends of these bones ensures the joint moves easily and without pain.
Indications for Elbow Replacement Surgery
- Severe Arthritis: Rheumatoid arthritis, osteoarthritis, and post-traumatic arthritis can lead to joint degeneration, causing severe pain and loss of function.
- Fractures: Complex fractures that cannot be repaired using other surgical methods may necessitate elbow replacement.
- Joint Instability: Chronic instability that cannot be managed through conservative treatments may require surgical intervention.
- Tumors: In rare cases, the presence of tumors in or around the elbow joint may require replacement surgery.
Types of Elbow Replacement Implants
There are several types of implants used in elbow replacement surgery, each designed to mimic the natural movement of the elbow joint:
Linked Implants
Linked implants are designed to mimic the natural hinge movement of the elbow. These implants are connected by a hinge mechanism, providing stability and reducing the risk of dislocation. They are typically recommended for patients with severe joint instability.
Unlinked Implants
Unlinked implants consist of two separate components that are not connected by a hinge. This design relies on the surrounding ligaments and muscles to provide joint stability. Unlinked implants are usually suitable for patients with intact ligaments and less severe joint damage.
The Surgical Procedure
Elbow replacement surgery involves several key steps:
Preoperative Preparations
Prior to surgery, the patient undergoes a thorough medical evaluation, including imaging studies such as X-rays and MRI scans. The surgeon discusses the procedure, potential risks, and expected outcomes with the patient.
Anesthesia
The surgery is performed under general anesthesia or regional anesthesia, depending on the patient’s health and the surgeon’s preference.
Incision and Exposure
An incision is made on the back of the elbow to expose the joint. The surgeon carefully removes the damaged cartilage and bone, preparing the area for the implant.
Implant Placement
The artificial components, typically made of metal and plastic, are positioned and secured in the humerus and ulna. The components are designed to fit together, allowing smooth joint movement.
Closure and Recovery
The incision is closed with sutures or staples, and the arm is placed in a splint or cast to protect the joint during the initial healing phase.
Postoperative Care and Recovery
Recovery from elbow replacement surgery involves several stages:
Hospital Stay
Patients typically stay in the hospital for a few days following the surgery. Pain management, infection prevention, and initial physical therapy exercises are initiated during this time.
At-Home Recovery
Once discharged, patients continue their recovery at home. Pain medications, wound care, and physical therapy are essential components of at-home care. It is crucial to follow the surgeon’s instructions and attend follow-up appointments to monitor the healing process.
Physical Therapy
Physical therapy is a vital part of the recovery process. Therapists work with patients to restore range of motion, strength, and flexibility in the elbow. Adhering to the prescribed therapy regimen greatly enhances the chances of a successful recovery.
Long-Term Care
Patients must maintain a healthy lifestyle and avoid activities that may stress the new joint. Regular check-ups with the surgeon are necessary to ensure the implant remains in good condition.
Potential Risks and Complications
Like any surgical procedure, elbow replacement surgery carries certain risks:
- Infection: Infections can occur at the incision site or within the joint.
- Nerve Damage: There is a risk of nerve injury during the procedure, which may result in numbness or weakness.
- Implant Issues: Loosening, dislocation, or wear of the implant components may occur over time.
- Blood Clots: Surgery increases the risk of developing blood clots in the veins.
Benefits of Elbow Replacement Surgery
Elbow replacement surgery can significantly improve the quality of life for individuals suffering from severe joint pain and dysfunction:
- Pain Relief: The surgery effectively reduces or eliminates chronic pain in the elbow joint.
- Improved Function: Patients experience enhanced joint mobility and strength, allowing them to perform daily activities with ease.
- Enhanced Quality of Life: Reduced pain and improved function contribute to a better overall quality of life.
Nursing Care of Patient with Elbow Replacement Surgery
Elbow replacement surgery is a sophisticated procedure aimed at alleviating severe joint pain and restoring function in patients with debilitating elbow conditions. This document outlines the essential nursing care considerations for patients undergoing elbow replacement surgery, ensuring an optimal recovery process.
Preoperative Care
Patient Education
Prior to surgery, it is crucial to educate the patient about the procedure, potential risks, benefits, and the postoperative care plan. This helps to alleviate anxiety and establish realistic expectations.
Health Assessment
Conduct a thorough health assessment, including medical history, current medications, and any allergies. Assess the patient’s cardiovascular, respiratory, and renal functions to ensure they are fit for surgery.
Preoperative Instructions
Provide the patient with clear instructions regarding fasting, medication adjustments, and pre-surgical hygiene practices. Emphasize the importance of adhering to these guidelines to minimize complications.
Postoperative Care
Pain Management
Effective pain management is essential for patient comfort and recovery. Administer prescribed analgesics, and monitor the patient for any adverse reactions. Encourage the use of non-pharmacological pain relief methods, such as ice packs and relaxation techniques.
Wound Care
Monitor the surgical site for signs of infection, such as redness, swelling, or discharge. Keep the incision clean and dry, and follow the surgeon’s guidelines for dressing changes. Educate the patient on proper wound care techniques to prevent infection.
Monitoring for Complications
Infection
Regularly check the incision site and monitor the patient’s temperature for signs of infection. If an infection is suspected, notify the healthcare provider immediately and follow the appropriate treatment protocol.
Nerve Damage
Assess the patient’s sensation and motor function in the affected arm and hand. Report any numbness, tingling, or weakness to the surgeon promptly.
Implant Issues
Monitor for signs of implant loosening or dislocation, such as unusual pain, swelling, or a clicking sensation in the joint. If these symptoms occur, advise the patient to avoid using the affected arm and seek medical attention.
Blood Clots
Encourage the patient to perform gentle movements and exercises to promote blood circulation and reduce the risk of blood clots. Administer anticoagulant medications as prescribed, and educate the patient on recognizing symptoms of deep vein thrombosis (DVT).
Physical Therapy
Physical therapy is a vital component of the recovery process, helping to restore joint function and strength. Collaborate with the physical therapist to develop a personalized rehabilitation plan for the patient. Encourage adherence to the prescribed exercises and monitor progress.
Patient Education and Support
Activity Restrictions
Instruct the patient on any activity restrictions, such as avoiding heavy lifting or repetitive arm movements. Provide guidance on how to perform daily activities safely to prevent strain on the new joint.
Follow-Up Appointments
Emphasize the importance of attending all follow-up appointments with the surgeon and physical therapist. These visits allow for monitoring of the patient’s progress and timely intervention if complications arise.
Emotional Support
Recovering from elbow replacement surgery can be challenging both physically and emotionally. Offer emotional support and encourage the patient to express any concerns or fears. Connect them with support groups or counseling services if needed.
REFERENCES
- American Academy of Orthopaedic Surgeons. Total Elbow Replacement. https://orthoinfo.aaos.org/en/treatment/total-elbow-replacement/. Last reviewed 4/2022.
- Arthritis Foundation. Elbow Surgery Options. https://www.arthritis.org/health-wellness/treatment/joint-surgery/preplanning/elbow-surgery-options).
- Davey MS, et al. Long-term outcomes of total elbow arthroplasty: A systematic review of studies at 10-year follow-up. Journal of Shoulder and Elbow Surgery. 2021; doi:10.1016/j.jse.2020.11.014.
- Evans JP, Evans JT, Mohammad HR, et al. How long does an elbow replacement last? A systematic review and meta-analysis of case-series and national registry reports with more than 10 years of follow-up (https://pubmed.ncbi.nlm.nih.gov/35642497/). Acta Orthop. 2022;93:495-502. Published 2022 May 31.
- Azar FM, et al. Shoulder and elbow arthroplasty. In: Campbell’s Operative Orthopaedics. 14th ed. Elsevier; 2021. https://www.clinicalkey.com.
- National Library of Medicine (U.S.). Elbow replacement (https://medlineplus.gov/ency/article/007258.htm). Last reviewed 9/20/2022.
- Total elbow replacement. American Academy of Orthopaedic Surgeons. https://orthoinfo.aaos.org/en/treatment/total-elbow-replacement. Feb. 15, 2022.
- Pooley J. Total elbow replacement – patient selection and perspectives (https://pubmed.ncbi.nlm.nih.gov/31040724/). Orthop Res Rev. 2019 Jan 25;11:23-40.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





