Transoral Robotic Surgery (TORS) represents a significant advancement in the field of minimally invasive surgery, especially within the realm of head and neck oncology. By leveraging the precision and flexibility of robotic technology, TORS has opened new possibilities for the treatment of complex anatomical regions that were once accessible only through highly invasive procedures.
History and Development of TORS
The origins of robotic-assisted surgery can be traced to the late 20th century, with initial applications in urology and cardiac surgery. The da Vinci Surgical System, developed by Intuitive Surgical, received FDA approval in 2000 and quickly became the platform of choice for robotic procedures.
The concept of applying robotic surgery transorally—through the mouth—emerged in the mid-2000s. Dr. Gregory Weinstein and Dr. Bert O’Malley at the University of Pennsylvania are credited with pioneering TORS in 2004. Their work culminated in FDA approval in 2009 for the use of robotic systems in the resection of benign and malignant tumors of the oropharynx.
The TORS Procedure: Overview and Process
Transoral Robotic Surgery utilizes a computer-enhanced surgical system to provide surgeons with enhanced visualization, dexterity, and precision. The essential components of a TORS procedure include:
- Robotic Platform: The da Vinci Surgical System is the most widely used system, consisting of a surgeon’s console, a patient-side cart with robotic arms, and a high-definition 3D vision system.
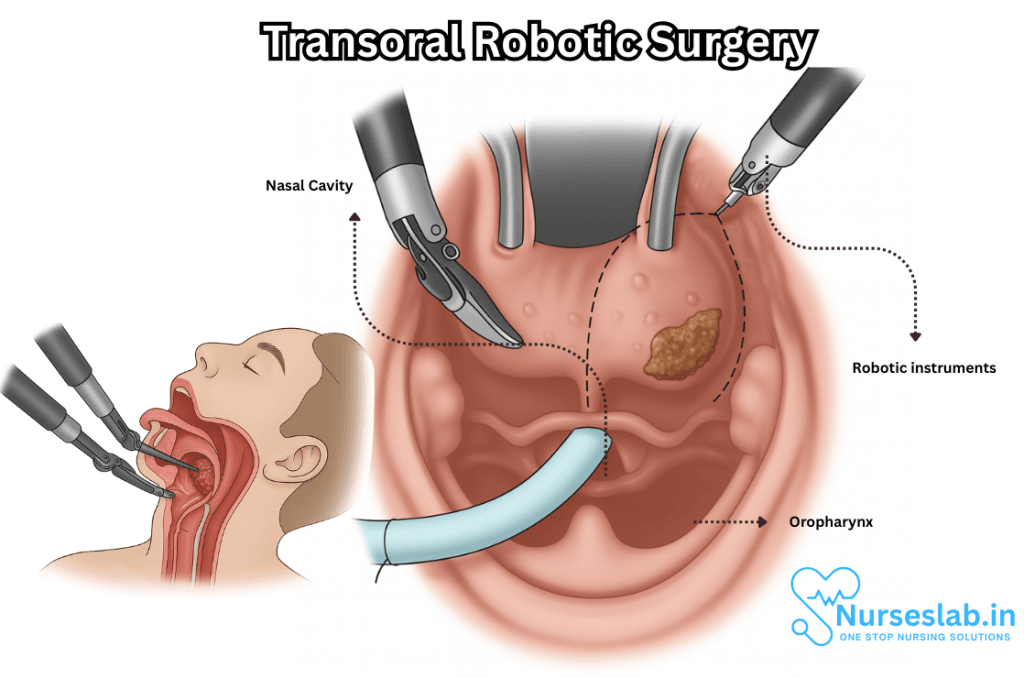
- Access: Unlike traditional open surgeries that require external incisions, TORS is performed entirely through the mouth, utilizing specialized retractors to provide access to the oropharyngeal cavity.
- Visualization: The system provides a magnified, three-dimensional view of the surgical field, allowing for meticulous identification of tumors and critical structures.
- Instrumentation: Miniaturized surgical instruments attached to the robotic arms are controlled remotely by the surgeon, who manipulates them with high precision via ergonomic controls at the console.
- Resection: The surgeon carefully removes the tumor and, if necessary, surrounding tissues, while preserving critical nerves and blood vessels.
Clinical Applications of TORS
Though initially developed for the oropharynx, the indications for TORS have expanded rapidly. The most common clinical applications include:
- Oropharyngeal Cancer: Tumors of the tonsil, base of tongue, and soft palate.
- Supraglottic Laryngeal Cancer: Tumors located above the vocal cords.
- Benign Lesions: Such as obstructive sleep apnea due to lingual tonsillar hypertrophy, cysts, or papillomas.
- Unknown Primary Tumors: Identification and resection of occult tumors in patients with cervical lymph node metastases of unknown origin.
- Reconstructive Surgery: Assisting in the repair and reconstruction of defects following tumor resection.
Advantages of TORS
TORS offers a range of benefits over traditional open or transoral non-robotic techniques:
- Minimally Invasive: TORS avoids large external incisions and extensive tissue disruption, resulting in faster recovery and decreased morbidity.
- Enhanced Visualization: Three-dimensional, high-definition magnified views help surgeons distinguish between tumor and healthy tissue.
- Precision and Dexterity: Robotic instruments articulate with greater range and steadiness than the human hand, enabling fine dissection in tight spaces.
- Reduced Hospital Stay: Many patients benefit from shorter hospitalization and a quicker return to normal activities.
- Better Functional Outcomes: TORS has been associated with improved speech and swallowing outcomes when compared with open surgeries or chemoradiation alone.
- Oncological Control: Studies suggest that TORS achieves comparable or better tumor control than traditional approaches, especially in early-stage oropharyngeal cancers.
Limitations and Challenges
Despite its many advantages, TORS is not without limitations:
- Patient Selection: Not all tumors are accessible or resectable using TORS, especially those involving the posterior pharyngeal wall or deeply infiltrating structures.
- Learning Curve: Surgeons require specialized training and experience to safely and effectively perform TORS.
- Equipment Cost: The acquisition and maintenance of robotic surgical systems are expensive, potentially limiting widespread adoption.
- Anesthesia and Airway Management: Operating in the upper aerodigestive tract poses unique challenges for anesthesiologists, including airway obstruction and bleeding risks.
- Long-Term Data: While early results are promising, more data is needed on long-term oncologic outcomes and quality of life.
Typical Patient Journey: Before, During, and After TORS
Preoperative Assessment: Patients undergo a thorough evaluation, including imaging (CT, MRI, or PET scans), endoscopic examination, and sometimes biopsy. A multidisciplinary team reviews each case to determine suitability for TORS.
Surgical Procedure: Under general anesthesia, the surgical team positions the patient and uses specialized retractors to expose the target area. The robotic arms are introduced transorally, and the surgeon operates from the console, removing the tumor with precision instruments.
Postoperative Care: Most patients are monitored in the hospital for 1-3 days. Pain is usually less than with open surgery, and many patients resume oral intake quickly. Speech and swallowing therapy may be recommended, depending on the extent of resection.
Follow-up: Regular follow-up appointments are scheduled to monitor healing, function, and recurrence. Adjuvant therapy (radiation or chemotherapy) may be recommended depending on pathology results.
Outcomes and Evidence
Multiple studies have demonstrated the safety and efficacy of TORS for early-stage oropharyngeal cancers. Key findings include:
- Oncological Outcomes: Comparable or improved survival rates relative to traditional surgery or chemoradiation in select patient populations.
- Functional Results: High rates of organ and function preservation, including speech and swallowing.
- Quality of Life: Many patients report better quality of life due to less pain, faster recovery, and fewer long-term complications.
Future Directions and Innovations
The evolution of TORS continues as technology and surgical expertise advance:
- Next-Generation Robots: Emerging platforms offer improved instrument maneuverability, smaller footprints, and even greater visualization capabilities.
- Expanded Indications: Research is ongoing into TORS applications for other regions, such as the hypopharynx, larynx, and skull base.
- Integration with Imaging: Real-time image guidance, augmented reality overlays, and enhanced navigation systems may improve accuracy and safety.
- Telemedicine and Remote Surgery: The potential for remote robotic surgeries could expand access to TORS expertise worldwide.
Nursing Care of Patients Undergoing Transoral Robotic Surgery (TORS)
The unique approach and anatomical site necessitate specialized nursing care to address specific risks, including airway compromise, bleeding, dysphagia, and infection.
Preoperative Nursing Care
Patient Assessment and Preparation
- Baseline Evaluation: Assess patient’s medical, surgical, and anesthetic history. Pay particular attention to comorbidities such as obstructive sleep apnea, cardiovascular disease, and bleeding disorders.
- Airway Assessment: Evaluate airway anatomy and potential difficulties in airway management. Collaborate with anesthesia and surgical teams to plan for possible airway interventions.
- Oral and Dental Health: Inspect for dental issues, loose teeth, or oral infections that may complicate access or healing post-surgery.
- Laboratory and Imaging: Ensure completion of necessary labs (CBC, coagulation profile) and imaging studies (CT, MRI, endoscopy).
Preoperative Education
- Explain the procedure, including what to expect before, during, and after surgery.
- Discuss potential complications such as bleeding, airway obstruction, swallowing difficulties, and voice changes.
- Provide instructions regarding fasting, medication adjustments (e.g., anticoagulants), and cessation of smoking or alcohol.
- Address concerns regarding pain, nutrition, and communication post-surgery.
Intraoperative Nursing Care
Operating Room Preparation
- Ensure availability and functionality of robotic surgical systems and backup equipment.
- Prepare standard and specialized instruments for airway access, suction, and hemostasis.
- Maintain a sterile field and assist with robotic docking and patient positioning (usually supine with the head extended).
Patient Monitoring
- Monitor vital signs, oxygen saturation, and end-tidal CO2 continuously.
- Assist anesthesia with airway management; be prepared for rapid intervention in case of airway compromise.
- Document intraoperative events, estimated blood loss, and any complications.
Postoperative Nursing Care
Immediate Postoperative Period
- Airway Management: Closely monitor for airway obstruction due to edema, hematoma, or secretions. Be prepared for emergency airway intervention (intubation, tracheostomy) if required.
- Pain Control: Administer prescribed analgesics, favoring non-opioid medications when possible to reduce sedation and risk of airway compromise. Use patient-controlled analgesia (PCA) if appropriate.
- Hemorrhage Surveillance: Check for signs of bleeding (oral cavity, pharynx, drains). Monitor for tachycardia, hypotension, or pallor, and report any abnormalities immediately.
- Swallowing and Aspiration Risk: Assess for dysphagia or signs of aspiration. Keep the patient NPO (nothing by mouth) until the surgical team authorizes oral intake, usually after a bedside swallow evaluation.
- Communication Support: Provide alternative methods for communication (writing boards, communication apps) if speech is impaired.
- Monitoring and Documentation: Record vital signs, neurological status, fluid intake/output, and wound assessment according to protocol.
Ongoing Postoperative Care
- Oral Care: Maintain meticulous oral hygiene to reduce risk of infection. Use non-alcoholic mouthwashes and gentle oral suction as needed.
- Nutritional Support: Collaborate with dietitians to advance the patient’s diet safely. Initiate tube feeds if prolonged NPO status is anticipated.
- Mobility and Activity: Encourage early mobilization to prevent venous thromboembolism, unless contraindicated.
- Pain and Symptom Management: Reassess pain regularly and adjust medications as needed. Monitor for nausea, vomiting, or constipation secondary to analgesics.
- Psychosocial Support: Provide reassurance and psychological support as patients may experience anxiety or depression due to altered appearance, speech, or swallowing.
- Education on Wound and Drain Care: Teach patients and caregivers about signs of infection, bleeding, or tube displacement if present.
Airway Vigilance and Emergency Response
- Continue to monitor for late-onset airway compromise, which may occur due to delayed swelling or hematoma formation.
- Ensure emergency airway equipment (suction, intubation tray, tracheostomy set) is immediately available at the bedside at all times, especially within the first 24-48 hours postoperatively.
Discharge Planning and Home Care
- Patient and Family Education: Provide comprehensive instructions on oral care, wound management, medication adherence, hydration, and nutrition.
- Signs of Complications: Instruct to watch for and promptly report symptoms such as difficulty breathing, bleeding, fever, severe pain, or signs of infection.
- Speech and Swallowing Therapy: Refer to speech-language pathologists as needed for ongoing rehabilitation.
- Follow-Up: Arrange for timely post-discharge follow-up with the surgical, oncology, and allied health teams.
Potential Complications and Nursing Interventions
- Airway Obstruction: Elevate the head of bed, apply humidified oxygen, and alert medical team immediately if stridor, dyspnea, or cyanosis occurs.
- Bleeding: Monitor closely for oozing or frank hemorrhage from the mouth. Apply gentle pressure if accessible; otherwise, activate emergency protocols.
- Infection: Observe for swelling, redness, pus, or fever. Adhere strictly to infection control practices.
- Swallowing Dysfunction: Collaborate with speech therapists and ensure safe feeding practices to prevent aspiration pneumonia.
- Voice Changes: Assess for hoarseness or loss of voice; provide communication aids as necessary.
Patient Education and Rehabilitation
Education is a cornerstone of postoperative care. Nurses play a key role in empowering patients and their families to participate actively in recovery. This includes:
- Clear explanations of the surgical site, anticipated changes in function, and the importance of monitoring for complications.
- Guidance on gradual reintroduction of oral intake, emphasizing small, soft meals and adequate hydration.
- Instructions regarding medication regimen, the importance of completing antibiotics, and pain management strategies.
- Referral to support groups or counseling services for psychological and emotional adjustment.
Interdisciplinary Collaboration
Optimal outcomes after TORS require active collaboration with a multidisciplinary team, including:
- Surgeons (Otolaryngology, Head & Neck Surgery)
- Anesthesiologists
- Speech and Swallowing Therapists
- Dietitians
- Oncologists (if cancer diagnosis)
- Social Workers and Psychologists
Nurses serve as the linchpin of this team, ensuring coordinated care, effective communication, and holistic support throughout the perioperative journey.
REFERENCES
- American Cancer Society. Cancer Facts and Figures 2023. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2023/2023-cancer-facts-and-figures.pdf.
- Baptista PM, Diaz Zufiaurre N, Garaycochea O, et al. TORS as Part of Multilevel Surgery in OSA: The Importance of Careful Patient Selection and Outcomes. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8878188/. J Clin Med. 2022;11(4):990.
- Hawkins J, Ahmad I. Anaesthesia for transoral robotic surgery. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8847838/. BJA Educ. 2022;22(3):118-123.
- Mella MH, Chabrillac E, Dupret-Bories A, Mirallie M, Vergez S. Transoral Robotic Surgery for Head and Neck Cancer: Advances and Residual Knowledge Gaps. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10056198/. J Clin Med. 2023;12(6):2303.
- Niewinski P, Golusiński WJ. Current indications and patient selection for transoral robotic surgery in head and neck cancer – a brief review. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9319182/. Contemp Oncol (Pozn). 2022;26(2):91-96.
- Costello AJ, et al., eds. Transoral robotic surgery for obstructive sleep apnea surgery. In: Principles and Practice of Robotic Surgery. Elsevier; 2024. https://www.clinicalkey.com.
- Oliver JR, Persky MJ, Wang B, et al. Transoral robotic surgery adoption and safety in treatment of oropharyngeal cancers. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9446338/. Cancer. 2022;128(4):685-696.
- Nguyen AT, et al. Comparison of survival after transoral robotic surgery vs nonrobotic surgery in patients with early-stage oropharyngeal squamous cell carcinoma. JAMA Oncology. 2020; doi:10.1001/jamaoncol.2020.3172.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





