Chronic pain refers to persistent or recurrent pain lasting longer than three months, often linked to injury, inflammation, nerve damage, or chronic illness. Understanding its causes, assessment, and management is essential in nursing, rehabilitation, and clinical practice.
Introduction
Chronic pain is a complex and often misunderstood medical condition that affects millions of people across the world, including a significant portion of the population in the world. Unlike acute pain, which serves as a warning signal for injury or illness and usually resolves with healing, chronic pain persists for months or even years, often without a clear cause.
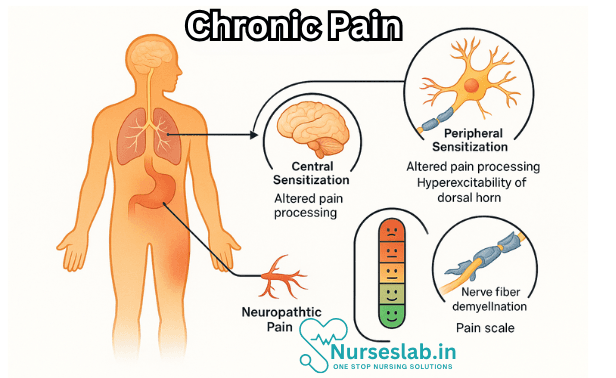
Defining Chronic Pain
Chronic pain is generally defined as pain that lasts longer than three to six months, or beyond the normal healing time for an injury. It can originate from various sources such as musculoskeletal disorders, nerve damage, or even without any identifiable physical cause. Chronic pain may be continuous or intermittent, and its intensity can range from mild discomfort to severe, debilitating agony.
Types of Chronic Pain Conditions
Chronic pain conditions encompass a wide spectrum of disorders. Some of the most common include:
- Chronic Back Pain: Often linked to degenerative disc disease, herniated discs, or spinal stenosis.
- Osteoarthritis: A degenerative joint disease causing persistent pain and stiffness.
- Rheumatoid Arthritis: An autoimmune disorder leading to joint inflammation and chronic pain.
- Fibromyalgia: Characterised by widespread musculoskeletal pain, fatigue, and sleep disturbances.
- Neuropathic Pain: Resulting from nerve damage, commonly seen in diabetes (diabetic neuropathy), shingles (postherpetic neuralgia), and sciatica.
- Chronic Headaches: Including migraines and tension-type headaches.
- Complex Regional Pain Syndrome (CRPS): A rare but severe pain condition affecting a limb, often following injury.
- Chronic Pelvic Pain: Seen in conditions like endometriosis or interstitial cystitis.
- Cancer-related Pain: Persistent pain associated with malignancies or their treatments.
Causes and Risk Factors
The causes of chronic pain are multifactorial and sometimes elusive. While some conditions have clear pathological origins, others may arise without any detectable injury or disease. Common causes and risk factors include:
- Previous Injuries: Inadequately healed fractures, sprains, or surgeries can lead to chronic pain.
- Medical Conditions: Diseases such as arthritis, diabetes, cancer, and autoimmune disorders are known contributors.
- Nerve Damage: Trauma, infections, or metabolic imbalances may result in neuropathic pain.
- Genetic Predisposition: Family history of chronic pain conditions increases risk.
- Psychological Factors: Stress, anxiety, and depression can both contribute to and exacerbate chronic pain.
- Lifestyle Factors: Sedentary behaviour, obesity, and poor posture are known risk enhancers.
- Age: Incidence increases with advancing age due to degenerative changes.
Impact of Chronic Pain
Chronic pain has profound effects on individuals, families, and society. Its impacts are not limited to physical suffering but extend to emotional, social, and economic domains.
- Physical Limitations: Persistent pain restricts mobility, leading to muscle weakness, joint stiffness, and reduced endurance.
- Emotional Toll: Chronic pain is often accompanied by depression, anxiety, irritability, and feelings of helplessness.
- Social Isolation: Sufferers may withdraw from social activities, resulting in loneliness and strained relationships.
- Economic Burden: Lost productivity, absenteeism, and increased medical expenses impose a significant financial strain on families and the healthcare system.
- Quality of Life: The overall life satisfaction and ability to enjoy daily activities diminish considerably.
Diagnosis of Chronic Pain Conditions
Diagnosing chronic pain is often challenging due to its subjective nature and the lack of specific biomarkers. A comprehensive approach usually involves:
- Detailed Medical History: Exploration of pain characteristics (location, duration, intensity), previous illnesses, and psychosocial factors.
- Physical Examination: Assessment of movement, tenderness, swelling, and neurological function.
- Imaging Studies: X-rays, MRI, CT scans may help identify structural abnormalities.
- Laboratory Tests: Blood tests to rule out infections, autoimmune diseases, or metabolic disorders.
- Psychological Assessment: Screening for depression, anxiety, and coping mechanisms.
- Pain Diaries: Patients may be asked to maintain records of pain episodes, triggers, and alleviating factors.
Management Strategies for Chronic Pain
Effective management of chronic pain requires a multifaceted approach, tailored to the individual’s needs and underlying causes. The following strategies are commonly employed:
Pharmacological Treatments
- Analgesics: Paracetamol and non-steroidal anti-inflammatory drugs (NSAIDs) are widely used for mild to moderate pain.
- Opioids: Reserved for severe pain, but their use is limited due to risk of dependence and side effects.
- Antidepressants: Drugs like amitriptyline and duloxetine are effective for neuropathic pain and fibromyalgia.
- Anticonvulsants: Gabapentin and pregabalin are beneficial in nerve-related pain.
- Topical Agents: Creams and patches containing capsaicin or lidocaine may provide local relief.
Physical Therapy and Rehabilitation
- Exercise Programmes: Tailored stretching, strengthening, and aerobic exercises help improve mobility and reduce pain.
- Manual Therapy: Physiotherapists use massage, mobilisation, and manipulation techniques.
- Electrotherapy: Techniques like transcutaneous electrical nerve stimulation (TENS) can modulate pain signals.
- Occupational Therapy: Focuses on enhancing daily function and adapting activities to minimise pain.
Psychological and Behavioural Interventions
- Cognitive Behavioural Therapy (CBT): Helps patients reframe negative thought patterns and develop coping strategies.
- Mindfulness and Meditation: Practices that foster relaxation and stress reduction.
- Biofeedback: Teaches control over physiological responses to pain.
- Support Groups: Peer interaction provides emotional support and shared experiences.
Interventional Procedures
- Nerve Blocks: Injection of anaesthetics or steroids around nerves to interrupt pain signals.
- Spinal Cord Stimulation: Implantable devices deliver electrical impulses to the spinal cord.
- Radiofrequency Ablation: Uses heat to disable pain-causing nerves.
- Trigger Point Injections: Relief for muscle-related pain syndromes.
Complementary and Alternative Therapies
- Ayurveda: Traditional Indian medicine utilises herbal remedies, dietary modifications, and yoga.
- Acupuncture: Insertion of fine needles at specific body points to relieve pain.
- Homeopathy: Individualised remedies based on symptom patterns.
- Yoga and Pranayama: Mind-body practices that improve flexibility, strength, and mental wellbeing.
Living with Chronic Pain: Practical Tips
Managing chronic pain is a lifelong journey requiring resilience, adaptability, and support. Here are some practical tips for individuals living with chronic pain:
- Maintain a Regular Routine: Consistency in daily activities fosters stability and predictability.
- Stay Active: Gentle movement is better than complete rest; consult your healthcare provider for appropriate exercises.
- Monitor Your Pain: Keep a diary to track patterns, triggers, and effective interventions.
- Seek Support: Connect with family, friends, or support groups to share experiences and reduce isolation.
- Practice Stress Management: Techniques such as meditation, yoga, and deep breathing can alleviate pain flare-ups.
- Educate Yourself: Understanding your condition empowers you to make informed choices.
- Communicate with Healthcare Providers: Open dialogue ensures better treatment outcomes and adjustments as needed.
Nursing Care of Patients with Chronic Pain
For nurses, the care of patients with chronic pain requires not only an understanding of pain mechanisms and pharmacological interventions but also a commitment to holistic care, communication, advocacy, and ongoing patient support.
Roles and Responsibilities of Nurses
Nurses play a pivotal role in the multidisciplinary management of chronic pain. Their responsibilities encompass assessment, planning, implementation, evaluation, education, support, and advocacy.
- Assessment: Comprehensive and ongoing evaluation of pain and its impact on the individual.
- Planning: Collaborating with the patient, healthcare team, and family to create a personalized pain management plan.
- Implementation: Administering pharmacological and non-pharmacological interventions, monitoring effects and side effects.
- Evaluation: Regularly reassessing pain and adjusting the care plan accordingly.
- Education: Teaching patients and families about pain, management options, self-care, and realistic expectations.
- Advocacy: Ensuring patient rights, access to appropriate pain management, and combating stigma around chronic pain.
Assessment of Chronic Pain
A thorough pain assessment is vital to effective pain management. This process begins with establishing trust and encouraging open communication.
Subjective Assessment
- Use validated pain assessment tools (e.g., Numeric Rating Scale, Visual Analog Scale, McGill Pain Questionnaire) to determine intensity and quality.
- Ask about onset, location, duration, character, aggravating and relieving factors.
- Explore how pain affects mood, sleep, mobility, activities of daily living, and social interactions.
- Assess coping mechanisms, beliefs about pain, and goals for treatment.
Objective Assessment
- Observe for behavioral cues (e.g., grimacing, guarding, decreased activity).
- Monitor vital signs, although these may not always correlate with chronic pain.
- Assess for side effects of analgesic therapy (e.g., sedation, constipation, respiratory depression).
- Evaluate physical limitations, joint mobility, muscle strength, and neurological status.
Pharmacological Interventions
Medication is a cornerstone of chronic pain management, tailored to the type and severity of pain, patient comorbidities, and responses.
- Non-Opioid Analgesics: Acetaminophen, NSAIDs (useful for mild to moderate nociceptive pain).
- Opioid Analgesics: Reserved for moderate to severe pain or cancer-related pain; monitor closely for side effects and potential dependency.
- Adjuvant Therapies: Antidepressants (e.g., amitriptyline for neuropathic pain), anticonvulsants (e.g., gabapentin), muscle relaxants, topical agents.
- Other: Nerve blocks, epidural injections, or implantable devices (in select cases).
Nurses must carefully monitor effectiveness, educate patients about medication use, side effects, and the importance of adherence, and advocate for safe opioid stewardship.
Non-Pharmacological Interventions
Integrating non-pharmacological approaches is essential, often enhancing the effectiveness of medications and improving overall well-being.
- Physical Therapies: Exercise, stretching, physiotherapy, massage, heat/cold applications, hydrotherapy.
- Psychological Interventions: Cognitive-behavioral therapy, mindfulness, relaxation techniques, guided imagery, biofeedback.
- Occupational Therapy: Assistance with adaptive devices, energy conservation, and modification of home/work environments.
- Complementary Therapies: Acupuncture, yoga, tai chi, aromatherapy, music therapy.
- Social Support: Encouraging participation in support groups, spiritual care, and community resources.
Patient Education and Empowerment
Empowering patients with knowledge and self-management skills is a fundamental aspect of nursing care for chronic pain.
- Provide clear information about the nature and causes of chronic pain.
- Encourage realistic goal-setting and expectations regarding pain relief.
- Teach self-care strategies such as pacing activities, proper use of assistive devices, and medication management.
- Support adherence to treatment plans and follow-up appointments.
- Discuss the importance of sleep hygiene, nutrition, stress management, and activity modulation.
Psycho-Social Considerations
Chronic pain often leads to anxiety, depression, social isolation, and altered family roles. Nurses must assess for these issues and facilitate appropriate referrals.
- Screen for mood disorders and suicidal ideation.
- Encourage open communication with family members and support systems.
- Refer to counselors, psychologists, or psychiatric services as needed.
- Promote activities that foster a sense of purpose and connection.
Interdisciplinary Collaboration
Effective management of chronic pain necessitates teamwork among healthcare professionals.
- Work closely with physicians, physiotherapists, pharmacists, psychologists, occupational therapists, and social workers.
- Participate in case conferences and care planning meetings.
- Communicate changes in patient condition or response to treatment promptly.
Nursing Process Applied to Chronic Pain
The nursing process is a structured, evidence-based approach to guide care:
- Assessment: Gather subjective and objective data as outlined above.
- Nursing Diagnosis: Common diagnoses include chronic pain, impaired physical mobility, disturbed sleep pattern, ineffective coping, and risk for social isolation.
- Planning: Establish goals in collaboration with the patient (e.g., improved pain control, enhanced mobility, better sleep).
- Implementation: Employ pharmacological and non-pharmacological strategies, adjusting as needed.
- Evaluation: Continually reassess pain, function, and quality of life, modifying the care plan as necessary.
Ethical and Legal Considerations
Nurses must be aware of ethical and legal dimensions in chronic pain management.
- Respect patient autonomy and preferences regarding treatment options.
- Maintain privacy and confidentiality in all communications and records.
- Advocate for effective pain relief while adhering to legal requirements and institutional policies regarding controlled substances.
- Combat stigma and misconceptions about chronic pain and opioid use.
Documentation
Accurate and timely documentation is critical for quality care, legal protection, and effective communication.
- Record comprehensive pain assessments, interventions, patient responses, and communications with other team members.
- Document teaching provided and patient understanding.
- Note any adverse effects, changes in condition, or significant communications with family or other providers.
Challenges in Nursing Care
The complexities of chronic pain can present significant challenges to nurses, such as:
- Managing patients with multiple comorbidities and individualized pain experiences.
- Balancing effective pain relief with the risks of medication side effects or dependency.
- Addressing cultural, spiritual, and belief-based differences in pain perception and expression.
- Preventing burnout and compassion fatigue among nursing staff.
REFERENCES
- Dydyk AM, Conermann T. Chronic Pain. https://www.ncbi.nlm.nih.gov/books/NBK553030/. 2024 May 6. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-.
- National Center for Complementary and Integrative Health (U.S.). Chronic Pain: What You Need to Know. https://www.nccih.nih.gov/health/chronic-pain-what-you-need-to-know. Last updated 1/2023.
- Treister AK, Hatch MN, Cramer SC, Chang EY. Demystifying poststroke pain: from etiology to treatment. PM R. 2017;9(1):63–75. doi:10.1016/j.pmrj.2016.05.015
- Rikard SM, Strahan AE, Schmit KM, Guy GP Jr.. Chronic Pain Among Adults — United States, 2019-2021. https://www.cdc.gov/mmwr/volumes/72/wr/mm7215a1.htm#suggestedcitation. MMWR Morb Mortal Wkly Rep. 2023 Apr;72:379-385.
- Stretanski MF, Kopitnik NL, Matha A, Conermann T. Chronic Pain. 2025 Jun 23. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 31971706.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





