Introduction
Transurethral Resection of Bladder Tumor (TURBT) is a minimally invasive surgical procedure commonly used for the diagnosis, staging, and treatment of bladder cancer. Bladder cancer is among the most frequent cancers affecting the urinary tract, and TURBT plays a pivotal role in its management. This document provides an in-depth look at the TURBT procedure, including its indications, techniques, potential risks, post-operative care, and long-term outcomes.
Understanding Bladder Cancer
Bladder cancer typically originates from the urothelial cells that line the inside of the bladder. It is most commonly detected in adults over the age of 55, with risk factors including smoking, exposure to certain chemicals, chronic bladder irritation, and a family history of the disease. Early symptoms can include painless blood in the urine (hematuria), frequent urination, urgency, and discomfort during urination.
Types of Bladder Cancer
- Non-muscle-invasive bladder cancer (NMIBC): The most common type, confined to the inner layers of the bladder wall.
- Muscle-invasive bladder cancer (MIBC): More aggressive, invading deeper layers or muscle of the bladder wall.
What is TURBT?
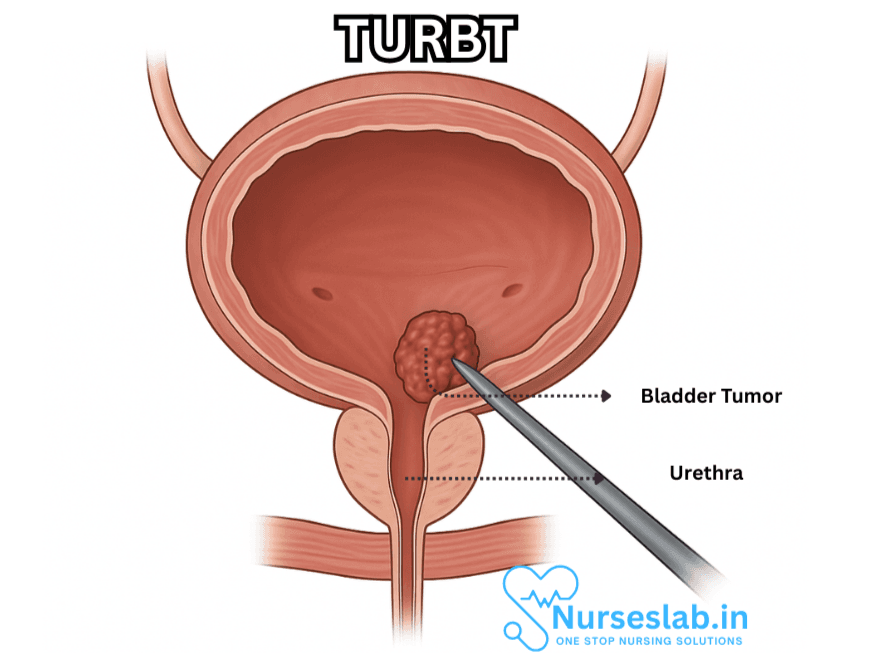
TURBT stands for Transurethral Resection of Bladder Tumor. It is both a diagnostic and therapeutic procedure that involves the removal of bladder tumors via the urethra using specialized instruments. Unlike open surgery, TURBT does not require external incisions, thus it offers a quicker recovery with less postoperative pain.
Indications for TURBT
TURBT is indicated in various clinical settings, including:
- Initial diagnosis of suspected bladder cancer detected via cystoscopy or imaging
- Treatment of visible bladder tumors, especially superficial and non-muscle-invasive lesions
- Re-staging or second-look procedures to assess for residual disease
- Management of recurrent bladder tumors
Preoperative Evaluation
Before undergoing TURBT, a thorough evaluation is conducted, including:
- Medical history and physical examination
- Urinalysis and urine cytology to detect malignant cells
- Imaging studies such as ultrasound, CT scan, or MRI to assess tumor size, location, and possible spread
- Blood tests to check kidney function, blood counts, and coagulation parameters
The TURBT Procedure
Anesthesia
TURBT is usually performed under regional (spinal or epidural) or general anesthesia, ensuring the patient is comfortable and pain-free during the operation.
Technique
The procedure involves the following key steps:
- Cystoscopy: A thin tube with a camera (cystoscope) is inserted through the urethra into the bladder to visualize the tumor(s).
- Tumor Resection: Using a resectoscope (a type of cystoscope equipped with a wire loop), the surgeon carefully removes the tumor tissue layer by layer. The goal is to entirely excise visible tumor tissue while minimizing damage to surrounding healthy tissue.
- Biopsy: Samples of the tumor and surrounding bladder tissue are collected for pathological analysis to determine the cancer grade and stage.
- Hemostasis: Bleeding is controlled using cauterization or other methods as needed.
- Bladder Irrigation: The bladder may be irrigated with saline to flush out blood clots and small tissue fragments, ensuring clear visualization and reducing the risk of post-operative complications.
Duration
The length of the procedure varies depending on the number, size, and location of tumors but typically ranges from 30 to 90 minutes.
Post-Operative Care
After TURBT, patients are closely monitored for any immediate complications. Key aspects of care include:
- Placement of a urinary catheter to drain urine and monitor for bleeding
- Continuous bladder irrigation may be used temporarily to prevent blood clot formation
- Pain management and monitoring for signs of infection
- Early mobilization to reduce the risk of blood clots in the legs (deep vein thrombosis)
Patients are generally able to resume normal activities within a few days, though it is advised to avoid heavy lifting and strenuous activity for several weeks.
Risks and Complications
Though TURBT is considered safe and effective, like any surgical procedure, it carries potential risks, including:
- Bleeding: Some blood in the urine is common, but significant bleeding may require intervention.
- Bladder perforation: Rarely, the bladder wall may be injured during resection.
- Infection: Risk of urinary tract infection or, less commonly, sepsis.
- Urinary retention: Temporary difficulty in urination post-surgery.
- Recurrence: Bladder tumors have a high rate of recurrence, necessitating regular follow-up.
Pathology Results and Staging
The tissue samples taken during TURBT are analyzed by a pathologist to determine:
- The type of bladder cancer (histology)
- The grade (how abnormal the cells appear under a microscope)
- The stage (how deeply the tumor has invaded the bladder wall)
This information is essential for planning further treatment and determining prognosis.
Additional Treatments
TURBT may be followed by adjuvant therapies to reduce the risk of recurrence and progression, especially for high-risk or recurrent tumors:
- Intravesical therapy: Instillation of medications directly into the bladder, such as Bacillus Calmette-Guérin (BCG) or chemotherapy agents like mitomycin C.
- Repeat TURBT: Sometimes needed if the initial resection is incomplete or if high-grade tumors are present.
- Radical treatments: For muscle-invasive cancers, radical cystectomy (removal of the bladder) and systemic chemotherapy may be recommended.
Follow-Up and Surveillance
Bladder cancer is notorious for recurrence. Therefore, careful surveillance is essential:
- Regular cystoscopic examinations to visually inspect the bladder
- Urine tests for cancer cells or tumor markers
- Imaging studies as indicated
The schedule and intensity of follow-up depend on the risk profile of the patient and the characteristics of the original tumor.
Benefits of TURBT
- Minimally invasive: No external incisions and relatively quick recovery
- Diagnostic and therapeutic: Both removes the tumor and provides tissue for diagnosis
- Repeatability: The procedure can be safely repeated in case of tumor recurrence
- Outpatient potential: Many patients can be treated without an overnight hospital stay
Limitations
- Recurrence risk: Bladder tumors may recur, necessitating lifelong surveillance
- Incomplete resection: Some tumors may not be entirely removed in one session
- Not suitable for all cancers: Muscle-invasive or advanced cancers often require additional interventions
Patient Experience and Recovery
Most patients experience mild urinary symptoms following TURBT, such as frequency, urgency, or mild discomfort. These typically resolve over time. Patients are encouraged to drink plenty of fluids, follow medication instructions, and contact healthcare providers if they notice persistent bleeding, fever, or severe pain.
Future Directions and Innovations
Advancements in endoscopic technology, imaging, and adjuvant therapies continue to improve the outcomes of TURBT. Enhanced visualization tools such as blue light cystoscopy and narrow-band imaging help detect smaller or less visible tumors, potentially reducing recurrence rates. Research into novel intravesical therapies and personalized approaches promises further improvements in the treatment of bladder cancer.
Nursing Care of Patients Undergoing Transurethral Resection of Bladder Tumor (TURBT)
Nursing care surrounding TURBT is multifaceted, encompassing the perioperative period, postoperative care, patient education, as well as monitoring for complications and long-term follow-up. This document details a holistic nursing approach to the care of patients undergoing TURBT.
1. Preoperative Nursing Care
Assessment and Preparation
- Comprehensive Assessment: Assess patient’s medical history, comorbid conditions (e.g., diabetes, coagulopathy, cardiovascular disease), current medications (especially anticoagulants), allergies, and previous surgeries.
- Baseline Investigations: Ensure laboratory tests (CBC, renal function, coagulation profile, urinalysis, urine culture) and imaging (ultrasound, CT, or MRI as indicated) are complete and reviewed.
- Informed Consent: Confirm that the procedure has been clearly explained by the physician and that informed consent has been obtained. Address any questions or concerns the patient may have.
Patient Preparation
- Fasting and Medication: Instruct the patient regarding preoperative fasting requirements and which medications to take or withhold (especially anticoagulants/antiplatelets). Ensure appropriate bridging if needed.
- Preoperative Hygiene: Encourage a thorough shower or bath before surgery. Shaving is generally not recommended to prevent microabrasions.
- Bladder Preparation: In some cases, the surgeon may order a bladder irrigation or antiseptic instillation preoperatively.
- Emotional Support: Provide psychological support; anxiety is common due to fear of cancer and surgery. Offer reassurance and answer questions honestly, encouraging patient or family involvement.
Education
- Procedure Explanation: Educate the patient about the TURBT procedure, the use of general or spinal anesthesia, and the expected duration of surgery.
- Expected Outcomes: Discuss the possible findings, need for repeat procedures, and the importance of follow-up cystoscopies.
- Postoperative Expectations: Prepare the patient for the presence of a urinary catheter, possible bladder irrigation, and the common occurrence of hematuria after surgery.
2. Intraoperative Nursing Care
Operating Room Preparation
- Patient Identification and Safety: Verify patient identity, allergies, and surgical site. Adhere strictly to surgical safety checklists.
- Positioning: Position the patient in the lithotomy position, ensuring proper padding to prevent nerve and pressure injuries.
- Aseptic Technique: Maintain strict aseptic technique to minimize the risk of infection.
- Monitoring: Assist anesthesia team in monitoring vital signs and ensuring patient comfort during the procedure.
Immediate Post-Procedure Tasks
- Specimen Handling: Ensure that resected tissue samples are correctly labeled and sent promptly to pathology.
- Documentation: Document intraoperative events, estimated blood loss, and any complications or deviations from the plan.
3. Postoperative Nursing Care
Immediate Postoperative Management
- Airway, Breathing, Circulation: On arrival in the recovery area, ensure the patient has a patent airway, stable vital signs, and adequate oxygenation.
- Pain Management: Assess pain level and administer analgesics as prescribed. Non-opioid options are preferable to minimize urinary retention.
- Urinary Output: Monitor closely for signs of obstruction or retention. The presence of a three-way Foley catheter for continuous bladder irrigation (CBI) is common to prevent clot formation.
- Hematuria: Expect blood in the urine initially, which should gradually clear over 24–72 hours. Monitor for persistent heavy bleeding or clot retention, and promptly notify the physician if these occur.
- Fluid Balance: Record input and output meticulously, including irrigation fluids. Assess for signs of fluid overload or electrolyte imbalance.
- Observation for Complications: Watch for signs of bladder perforation (abdominal pain, distension, peritonitis), infection (fever, dysuria), deep vein thrombosis, and anesthetic complications.
Catheter Care and Bladder Irrigation
- Catheter Maintenance: Ensure the catheter is patent, appropriately secured, and flowing freely. Irrigate gently if occluded by clots, and only as per protocol or order.
- Infection Prevention: Employ strict hand hygiene, maintain a closed system, and routinely inspect the catheter site for signs of infection.
- Patient Instruction: Explain the purpose of the catheter, expected duration, and instruct the patient not to pull or kink the tubing.
Pain and Discomfort Management
- Bladder Spasms: Anticholinergic medications may be prescribed for spasms. Provide comfort measures and reassurance.
- Analgesia: Use the least invasive pain management strategies. Assess pain regularly and intervene early.
Prevention of Deep Vein Thrombosis (DVT)
- Encourage early mobilization as soon as appropriate.
- Use compression stockings or intermittent pneumatic compression devices as ordered.
- Monitor for calf tenderness, swelling, or redness.
Nutrition and Hydration
- Once fully awake, encourage oral fluids unless contraindicated, to help flush residual blood and reduce infection risk.
- Resume diet as tolerated, typically beginning with clear liquids and progressing as per patient tolerance.
Psycho-Social Support
- Address feelings of anxiety or depression due to cancer diagnosis or fear of recurrence.
- Provide access to counseling, support groups, or oncology nurse navigators.
Patient and Family Education
- Signs of Complications: Teach the patient to recognize and seek immediate help for excessive bleeding, severe pain, fever, chills, or signs of infection.
- Catheter/Care at Home: If discharged with a catheter, instruct on care, emptying the bag, maintaining hygiene, and when to seek help.
- Activity Restrictions: Advise on avoiding heavy lifting, strenuous exercise, and driving until cleared by the physician.
- Follow-up: Stress the importance of attending scheduled cystoscopies and follow-up appointments for early detection of recurrence.
4. Discharge Planning and Long-Term Nursing Care
- Discharge Criteria: Stable vital signs, adequate pain control, clear urine or minimal hematuria, ability to void (if catheter-free), understanding of post-discharge care.
- Medications: Review all prescribed medications, including antibiotics, analgesics, and any intravesical therapy (e.g., BCG instillation) if applicable.
- Home Support: Assess for adequate home support, ability to care for catheter (if present), and access to emergency care if complications arise.
- Lifestyle Modifications: Counsel on smoking cessation and healthy lifestyle choices to reduce recurrence risk.
- Emotional and Psychological Care: Continue to offer support for adjustment, coping, and dealing with uncertainties of cancer diagnosis and treatment.
5. Monitoring and Complication Management
- Acute Complications: Include severe hematuria, clot retention, infection, urinary retention, and, rarely, bladder perforation. Early recognition and intervention are critical.
- Chronic Complications: These may include bladder fibrosis, contracture, or recurrence of tumor. Regular surveillance is key.
Key Signs to Report Immediately:
- Persistent heavy bleeding or clots
- Severe abdominal or pelvic pain
- Signs of infection (fever, chills, dysuria)
- Decreased urine output or inability to void
- Catheter malfunction or leakage
6. Special Considerations
- Elderly Patients: May have increased risk of complications due to comorbidities and frailty; require closer monitoring and tailored patient education.
- Recurrent Disease: Patients undergoing frequent TURBTs may experience anxiety or distress; continuous psychosocial support and education are essential.
- Intravesical Therapy: Some patients will require additional treatments such as BCG or chemotherapy after TURBT. Nurses must ensure these are administered safely and that patients are educated about side effects and precautions.
REFERENCES
- American Urological Association. What Is Non-Muscle Invasive Bladder Cancer?. https://www.urologyhealth.org/urology-a-z/n/non-muscle-invasive-bladder-cancer Updated 8/8/2020.
- Sun S, Wang H, Zhang X, Chen G. Transurethral Resection of Bladder Tumor: Novel Techniques in a New Era. Bladder (San Franc). 2023 Nov 9;10:e21200009. doi: 10.14440/bladder.2023.865. PMID: 38022709; PMCID: PMC10668603.
- Transurethral resection of a bladder tumor (TURBT) procedure. (2022).
https://bcan.org/bladder-cancer-turbt/ - Kim LHC, Patel MI. Transurethral resection of bladder tumour (TURBT). https://pubmed.ncbi.nlm.nih.gov/33457279/. Transl Androl Urol. 2020 Dec;9(6):3056-3072
- Trans urethral removal of bladder tumour (TURBT). (2022).
https://www.cancerresearchuk.org/about-cancer/bladder-cancer/treatment/non-muscle-invasive/trans-urethral-removal-tumour - Maltagliati M, Varca V, Milandri R, et al. Second-look TURBT: evaluation of anatomopatological and oncologic results in a single center. https://pubmed.ncbi.nlm.nih.gov/32420968/. Acta Biomed. 2020 May 11;91(2):322-325.
- Chen S, Xu R, Cheng Y, Wu J, Zhu X, Mahmoud O, Antar RM, Avudaiappan AP, Zhang J, Wang B, Chen Y. Clinical outcomes of modified partial cystectomy in muscle-invasive bladder cancer: balancing tumor control and quality of life. Transl Androl Urol. 2025 May 30;14(5):1444-1455. doi: 10.21037/tau-2025-243. Epub 2025 May 27. PMID: 40529028; PMCID: PMC12170104.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





