Introduction
Peritoneal dialysis (PD) stands as a vital lifeline for people living with kidney failure, offering an alternative to hemodialysis and, in some cases, a bridge to transplantation. Utilizing the natural lining of the abdomen—the peritoneum—this technique allows for the gentle and continuous removal of waste products and excess fluids from the blood. As chronic kidney disease (CKD) and end-stage renal disease (ESRD) continue to affect millions worldwide, understanding how peritoneal dialysis works, its advantages, limitations, and impact on patients’ lives is more important than ever.
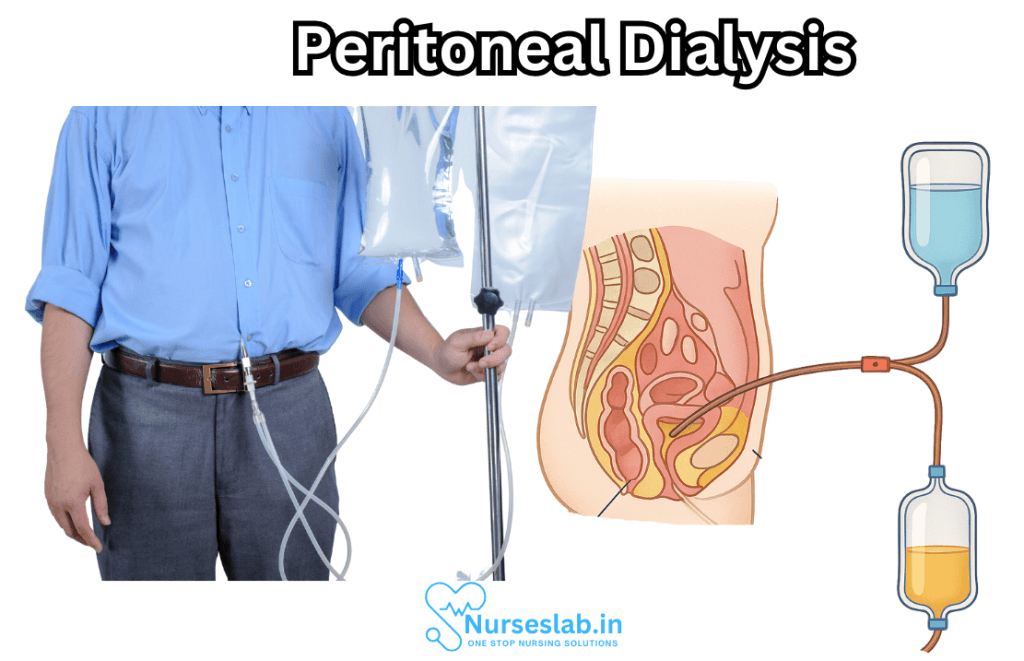
Understanding Peritoneal Dialysis
What is Peritoneal Dialysis?
Peritoneal dialysis is a medical procedure designed to cleanse the blood of toxins and to regulate fluid balance when the kidneys can no longer perform these functions effectively. The process hinges on the peritoneum—a semi-permeable membrane lining the abdominal cavity—which acts as a natural filter. A special dialysis solution, or dialysate, is infused into the peritoneal space, drawing waste and excess water from the blood through osmosis and diffusion.
Types of Peritoneal Dialysis
There are two primary forms of peritoneal dialysis:
- Continuous Ambulatory Peritoneal Dialysis (CAPD): This method does not rely on machinery. Instead, patients manually exchange the dialysate four to five times daily, allowing the fluid to dwell in the abdomen for several hours before draining and refilling. CAPD allows for flexibility and independence but requires adherence to strict technique and hygiene.
- Automated Peritoneal Dialysis (APD): Also known as continuous cycling peritoneal dialysis (CCPD), this method utilizes a machine (cycler) that performs multiple exchanges, typically overnight while the patient is asleep. APD can be more convenient for those with active lifestyles or children.
The Procedure: How Peritoneal Dialysis Works
Catheter Placement
PD begins with the insertion of a soft, flexible tube called a Tenckhoff catheter into the lower abdomen. This minor surgical procedure is usually performed under local anesthesia. The catheter provides ongoing access to the peritoneal cavity for the infusions and drains of dialysate.
The Exchange Process
Each treatment cycle, or “exchange,” has three phases:
- Fill: Sterile dialysate is introduced into the peritoneal cavity through the catheter.
- Dwell: The dialysate remains in the abdomen, allowing wastes and excess fluid to pass from the blood vessels in the peritoneal lining into the solution.
- Drain: After a set dwell time, the fluid—now containing wastes and extra water—is drained out and discarded, and a new cycle begins.
CAPD typically involves several daytime exchanges, while APD cycles are managed by a machine at night.
The Dialysate Solution
Dialysate is a sterile fluid composed mainly of water, electrolytes (like sodium, chloride, and calcium), and glucose or other osmotic agents. The composition can be adjusted to meet individual patient needs, such as controlling blood sugar or correcting electrolyte imbalances.
Advantages of Peritoneal Dialysis
- Greater Independence: Patients can self-administer PD at home or in other settings, reducing the need for frequent clinic visits.
- Flexibility: PD offers patients the freedom to tailor treatment around their schedules, making travel and work more manageable.
- Gentler on the Body: The continuous nature of PD is often less taxing on the heart and blood pressure than hemodialysis’ rapid fluid shifts.
- Preservation of Residual Kidney Function: Studies suggest PD may better maintain remaining kidney function compared to hemodialysis.
- Better for Children: Because of its gentle, continuous action, PD is often preferred for pediatric patients.
Challenges and Risks
Despite its benefits, peritoneal dialysis carries certain risks and drawbacks:
- Peritonitis: The most serious complication is infection of the peritoneal cavity, usually due to contamination during exchanges. Symptoms include abdominal pain, fever, and cloudy drainage fluid.
- Catheter-Related Issues: Blockage, leakage, or infections at the catheter site can occur.
- Weight Gain and Metabolic Changes: The glucose in dialysate can be absorbed, leading to weight gain and sometimes difficulties in diabetes management.
- Protein Loss: Some proteins are lost in the dialysate, potentially contributing to malnutrition.
- Not Suitable for All: Patients with previous extensive abdominal surgery, hernias, or inflammatory bowel disease may not be candidates for PD.
Comparing Peritoneal Dialysis and Hemodialysis
While both peritoneal dialysis and hemodialysis serve the same fundamental purpose, their approaches differ significantly:
- Location: PD is typically home-based, while hemodialysis is often performed in a clinic or hospital.
- Frequency: Hemodialysis is generally done three times a week, whereas PD is performed daily.
- Impact on Lifestyle: Many patients find PD less disruptive to their daily lives, though it requires commitment and aseptic technique.
- Medical Suitability: The choice depends on medical history, lifestyle, and personal preference. Some patients may switch modalities over time.
Training and Support
Transitioning to peritoneal dialysis involves comprehensive training from a multidisciplinary healthcare team. Patients and caregivers learn how to:
- Prepare and maintain a clean environment
- Perform exchanges safely
- Recognize signs of infection and other complications
- Care for the catheter
- Order and store supplies
Ongoing support is provided through regular clinic visits, blood tests to monitor treatment effectiveness, and 24/7 access to specialized PD nurses.
Living with Peritoneal Dialysis
Daily Routine
Patients incorporate exchanges into their daily routines, whether at home, work, or while traveling. Modern supplies and portable cyclers have made it possible for individuals to maintain active and fulfilling lives.
Diet and Lifestyle
Nutritional guidelines for people on PD usually include:
- Moderate protein intake to replace losses
- Careful monitoring of salt, potassium, and fluid intake
- Attention to calorie balance, especially given glucose absorption from dialysate
Patients are encouraged to remain physically active, avoid smoking, and manage other health conditions, such as hypertension and diabetes.
Emotional and Social Aspects
Coping with chronic illness and dialysis can be challenging. Many patients benefit from support groups, counseling, and open communication with their healthcare team and loved ones.
Nursing Care of Patients Undergoing Peritoneal Dialysis
The role of the nurse is paramount in ensuring the safety, comfort, and well-being of patients undergoing peritoneal dialysis. This guide provides an in-depth overview of nursing care for these patients.
Nursing Assessment
Initial Assessment:
- Review patient history, including reason for dialysis, comorbidities, and previous complications.
- Assess baseline vital signs, weight, and laboratory values (e.g., electrolytes, urea, creatinine).
- Evaluate the peritoneal dialysis access site for signs of infection, leakage, or displacement.
- Assess understanding of the dialysis process and ability to perform self-care.
Ongoing Monitoring:
- Monitor vital signs before, during, and after exchanges.
- Observe the patient for signs of complications, including infection, hypotension, and electrolyte imbalances.
- Monitor ultrafiltration volume and characteristics of effluent (clarity, color, presence of fibrin or blood).
- Regularly assess the access site for redness, swelling, pain, discharge, and healing.
- Evaluate patient’s nutritional status, fluid balance, and psychosocial well-being.
Infection Prevention and Control
The risk of infection, particularly peritonitis and exit-site infections, is a major concern in peritoneal dialysis. Nursing care focuses on strict aseptic techniques and patient education.
- Perform hand hygiene before and after handling dialysis equipment or touching the catheter site.
- Use sterile supplies for exchanges and ensure a clean environment.
- Educate patients and caregivers on hand hygiene, proper technique, and signs of infection (e.g., cloudy effluent, abdominal pain, fever, redness at the exit site).
- Regularly inspect the catheter exit site and reinforce the dressing as needed.
- Administer prophylactic antibiotics as prescribed (e.g., topical mupirocin at the exit site).
- Document and report any signs of infection immediately to the healthcare provider.
Dialysis Exchange Procedures
A nurse’s role includes both performing exchanges in the clinical setting and training patients for home-based care.
Preparation:
- Gather all necessary sterile equipment and supplies.
- Review the physician’s prescription for dialysate volume, dwell time, and additives.
- Ensure the patient’s comfort and privacy.
- Inspect dialysate for cloudiness, leaks, or contamination.
Exchange Process:
- Perform hand hygiene and don sterile gloves.
- Connect dialysate bags and tubing using aseptic technique.
- Clamp and unclamp lines as per protocol to instill and drain dialysate.
- Monitor patient for discomfort, pain, or unusual symptoms during the exchange.
- Upon completion, record the volume of effluent drained and compare with the volume instilled to assess ultrafiltration.
Post-Exchange Care:
- Dispose of used dialysate and materials following standard precautions.
- Reassess the patient’s vital signs and overall well-being.
- Ensure the catheter and exit site are clean, dry, and properly dressed.
- Document the procedure, findings, and any patient concerns or complications.
Patient and Family Education
Empowering patients and their families through education is vital for safe and effective home-based PD.
- Teach step-by-step techniques for performing exchanges, maintaining sterile conditions, and troubleshooting problems.
- Demonstrate care of the catheter and exit site, including cleaning and dressing changes.
- Explain the importance of regular monitoring of effluent and recognizing early signs of complications.
- Provide written materials and hands-on practice sessions to build competence and confidence.
- Discuss diet and fluid restrictions, emphasizing the importance of following prescribed regimens to avoid fluid overload and electrolyte imbalances.
- Encourage open communication with the healthcare team and provide contact information for questions or emergencies.
Nutritional and Fluid Management
Proper nutrition and fluid balance are integral to the success of peritoneal dialysis.
- Collaborate with a dietitian to tailor dietary recommendations based on individual needs.
- Monitor laboratory results for serum albumin, potassium, phosphorus, calcium, and glucose (especially in diabetic patients).
- Advise on adequate protein intake to prevent malnutrition, considering protein loss in dialysate.
- Guide on sodium and fluid restriction to prevent volume overload and hypertension.
- Educate about potential need for phosphate binders and vitamin supplementation.
Complications and Their Management
Complications of peritoneal dialysis can be acute or chronic, and prompt recognition and intervention are crucial.
Peritonitis
- Signs/Symptoms: Cloudy effluent, abdominal pain, fever, nausea, vomiting.
- Nursing Actions: Obtain effluent sample for culture, initiate prescribed antibiotics, monitor patient closely, reinforce aseptic technique, and educate on prevention.
Exit Site and Tunnel Infections
- Signs/Symptoms: Redness, swelling, tenderness, purulent discharge at catheter site.
- Nursing Actions: Clean and dress the site, administer topical or systemic antibiotics as ordered, monitor for spread of infection, and reinforce patient education.
Mechanical Complications
- Examples: Catheter blockage, leakage, hernias, dialysate retention.
- Nursing Actions: Assess catheter patency, reposition patient as needed, report persistent issues to the provider, and support patient during interventions.
Metabolic Complications
- Examples: Hyperglycemia (from glucose in dialysate), electrolyte imbalances, hypoproteinemia.
- Nursing Actions: Monitor blood glucose, electrolytes, and nutritional status; adjust medications or solutions as per medical advice.
Psychosocial Support
Chronic illness and home-based dialysis can be challenging emotionally and socially for patients and families.
- Assess coping strategies, mood, and support systems.
- Provide counseling or referrals to mental health services as needed.
- Encourage participation in support groups for patients on dialysis.
- Respect cultural, spiritual, and individual preferences in care.
Documentation and Communication
Accurate record-keeping and clear communication are essential for continuity of care.
- Document all assessments, procedures, patient responses, education provided, and any complications or interventions.
- Communicate changes in patient condition, concerns, or abnormal findings promptly to the multidisciplinary team.
REFERENCES
- Chaudhary K. Peritoneal Dialysis Drop-Out: Causes and Prevention Strategies. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3205769/. Int J Nephrol. 2011 Oct;2011:434608.
- Skorecki K, et al., eds. Peritoneal dialysis. In: Brenner & Rector’s The Kidney. 11th ed. Elsevier; 2020. https://www.clinicalkey.com.
- Merck Manuals, Consumer Version. Dialysis. https://www.merckmanuals.com/home/kidney-and-urinary-tract-disorders/dialysis/dialysis. Last reviewed/updated 7/2024.
- Feehally J, et al., eds. Peritoneal dialysis. In: Comprehensive Clinical Nephrology. 6th ed. Elsevier; 2019. https://www.clinicalkey.com.
- National Health Service (UK). Dialysis. https://www.nhs.uk/conditions/dialysis/. Last reviewed 9/29/2021.
- National Institute of Diabetes and Digestive and Kidney Diseases (U.S.). Peritoneal Dialysis. https://www.niddk.nih.gov/health-information/kidney-disease/kidney-failure/peritoneal-dialysis. Last reviewed 1/2018.
- National Kidney Foundation (U.S.). Multiple pages reviewed for this article. https://www.kidney.org/.
- National Library of Medicine (U.S.). Dialysis – Peritoneal. https://medlineplus.gov/ency/article/007434.htm. Last reviewed 10/19/2022.
Stories are the threads that bind us; through them, we understand each other, grow, and heal.
JOHN NOORD
Connect with “Nurses Lab Editorial Team”
I hope you found this information helpful. Do you have any questions or comments? Kindly write in comments section. Subscribe the Blog with your email so you can stay updated on upcoming events and the latest articles.





